
MIREBALAIS, Haiti (En français | En español) — Cervical cancer is a disease that Haiti cannot afford. And in most cases, it’s a disease the country’s broken healthcare system cannot treat.
There is just one MRI scanner in the entire country of 11 million people. Radiation treatment does not exist — for any kind of cancer — because there are no machines. Cancer screenings and early detection programs are limited, and so is access to lifesaving care.
In a country already struggling to manage maternal deaths and childhood diseases that have been largely controlled in other parts of the world, cervical cancer is nearly always a death sentence. Haitians who can afford to travel abroad for treatment are the few who have a fighting chance against advanced forms of the disease.
But cancer experts say it doesn’t have to be that way. Though cervical cancer is one of the leading causes of cancer deaths for women in Haiti, it is both preventable and treatable.

Estimates of the number of deaths caused by cervical cancer in Haiti vary widely, in part because people often die with no record of the cause. But healthcare providers in Haiti such as Partners in Health, a Boston-based nonprofit, put the number at 1,500 or more a year, basing their estimates on 10 years of data. The International Agency for Research on Cancer, the World Health Organization’s cancer arm, is far more conservative, saying an estimated 563 women will die from the disease in Haiti this year.
Even at the lower number, the mortality rate in Haiti is six times that of the United States.
Most of those deaths, researchers say, can be linked to poverty. In a country like Haiti, where most people live on less than $2 a day and many poor women often work as street vendors to keep families afloat, the deaths also have a ripple effect, sending more children to orphanages and accelerating the downward spiral of the already poor.
“These are unnecessary deaths that have great impact on individual families and the economy of our country,” said Didi Bertrand-Farmer, a Haitian healthcare advocate who is emerging as a leading voice in a campaign to reverse the deadly trend.
Bertrand-Farmer knows the disease well. At 14, she lost her mother to cervical cancer in Haiti, and later, as a community organizer in the African nation of Rwanda, she worked to help reduce the disease. The wife of acclaimed Partners In Health physician Paul Farmer, she is now part of a cervical cancer consortium formed by a group of U.S.-based doctors, called Haiti sans Cervical Cancer, to build a national prevention program.
“It is no longer acceptable for women in this country to keep dying from cervical cancer,” Bertrand-Farmer said. “My biggest concern is: How are we protecting the lives of the new generation of girls?”
‘I ALREADY KNOW I AM GOING TO DIE’
In Haiti, women carry the financial burden for their families. Called the poto mitan — the backbone of the society — they are wives and mothers but also ti-machans, or street merchants, who scratch out a living in the country’s informal economy.
When Paula Paul, 44, one of those street merchants, learned in April that she had cervical cancer, she had never been screened for the disease. She hadn’t heard of it and certainly wasn’t familiar with its cause, which is usually the human papillomavirus (HPV), a common sexually transmitted infection. The U.S. Centers for Disease Control and Prevention recommends getting two doses of the HPV vaccine as early as age 11.
The disease had advanced beyond the early stages. Had it been detected early, a hysterectomy or more minor surgery could have stopped the spread of the disease and most likely cured her.

But Paul had probably been living with cancer for at least five years. She had assumed the frequent, irregular vaginal bleeding, which started when her daughter, now 6, was a year old, was a side effect of her birth-control implant.
“I don’t know where it came from. I thought it was due to my family, but my family line doesn’t have it,” Paul said. “I don’t have anyone who has this disease.”
She said she has accepted that the illness will take her life: “I already know that I am going to die — what else is there for me to do?”
And yet it’s clear she hasn’t given up hope. After starting chemotherapy in May, she said, she expected to die quickly. Instead, she feels better. And even though the doctor said she shouldn’t exert herself, there are days when she feels up to lifting a bucket of water or hand-washing clothes.
“I’m not saying that I am cured but I used to bleed a lot before the medication and now I don’t bleed anymore,” she said. “When I go get my chemotherapy, the [doctors] say they are very happy and I should pray for all of my lab results to be the same way.”
Even more than about her health, though, she agonizes about what will happen to her children, especially her youngest, 6-year-old Marie Stacey.

Her family — a sister and a sick aunt live nearby, and her elderly mother is in Port-au-Prince — is too poor to care for her daughter after she dies, she has concluded. She’s considered handing the girl over to an orphanage to ensure Marie Stacey gets an education. Too sick to work and earn money for school fees, she was forced to pull the child from kindergarten, and has been unable to send her back to school.
During a trip in June to the University Hospital of Mirebalais in central Haiti, where she goes every 15 days for palliative care to ease the pelvic pain, Paul was blunt: “I’m by myself. I have nobody to help me.”
She’s mostly stoic, showing emotion only when she talks about her daughter. Even when chemotherapy quickly took her hair, she shrugged off any attempt at sympathy: “You can’t cry about hair.”
About three months into her treatment, her doctor prescribed pain pills to take three times a day — with food. But even that isn’t easy. She doesn’t have much money for food. The meager amount she had saved before the cancer is all gone, used to pay for transportation to the Mirebalais hospital, two hours away.
Before cancer, Paul supported herself and her children by selling dry goods in the Pond Sonde market near her two-room house in Bellanger, a rural community in Haiti’s Lower Artibonite Valley. She’d buy rice and spices in bulk, then sell individual portions at the market.
Now, just getting to the hospital for treatment can seem like an insurmountable obstacle. In August, five days before her upcoming chemotherapy appointment, she sat on her front porch and assessed the bleak situation. She had no money for the two-hour trek by bus or on the back of a motorcycle. She’d last eaten the day before, a plate of grits. And she didn’t have the $28 for three tests required before each chemo session, she said, pulling a piece of paper with the tests written on it from the pages of her Bible.
Normally, the tests are free at the Mirebalais hospital, a $16 million facility built by Partners In Health that provides free healthcare to more than 1,000 patients a day.. But this time, the CT scanner was broken when Paul needed a scan to see how the treatment was working. Patients had to go to a private lab and pay for exams.
Or, as in Paul’s case, skip a treatment.
“I don’t have any money,” she said. “Everything I had to sell, I sold.”
As she discussed the treatment she couldn’t afford, Paul could hear the sounds of life going on around her. Music blared occasionally from down the street, drowning out boisterous laughter from a group of young men playing dominoes just beyond her front gate. Her yard was mostly dirt with a lone mango tree, long since stripped of its fruit.
Her daughter, who had been playing with a neighbor’s son, ran through the gate and flashed a shy grin. Seeing Marie Stacey, Paul tried to focus on the words of a private doctor who told her the cancer was operable and the Mirebalais physician who said the cancer had not yet entered her bloodstream.
“I’m thinking,” Paul said, almost to herself, “how did I discover a disease early and yet I can’t get treated for it?”
COUNTING CASES
In Haiti, as in most poor countries, cancer is such a neglected health problem that the government doesn’t even know how many cancer patients there are, much less the number of new diagnoses.
But Robert Auguste, a gynecologist and former health minister, is trying to change that.
For the past five years, Auguste — who heads the government’s National Cancer Registry — has traveled the country three times a year in a beat-up 2006 Nissan Patrol to personally collect reports on all cancers because regional health ministers sometimes “don’t even respond” to his requests for monthly numbers.
“They don’t understand the importance,” he said.
Auguste does. He served as Haiti’s health minister in 2006 and advocated for construction of Haiti’s first center for radiotherapy, chemotherapy and nuclear medicine.
The government only got as far as approving a $10 million budget item and laying an official cornerstone in Port-au-Prince across the street from the State University of Haiti Hospital, also known as the General Hospital, before the idea was abandoned in the wake of the 2010 earthquake. Today, even the stone has disappeared under a pile of rocks and garbage.
Today, there are just three places in Haiti where middle-class and poor people have any hope of getting cancer care they can afford: the General Hospital, the Partners in Health hospital in Mirebalais or the treatment center run by the nonprofit Innovating Health International. None have radiation treatment.
That leaves most cancer patients with few options. “Everybody can’t go to Cuba. Everybody can’t go to the Dominican Republic. Everybody can’t go to the United States,” Auguste said.
It wasn’t always like this. During the nearly 30-year-long Duvalier family dictatorship, Haiti had radiation, also known as radiotherapy. But when the dictatorship fell in 1986, radiation therapy, like many services, disappeared due to lack of money. Today, those who study the incidence of cancer are certain that Haiti’s inability to offer such treatment for cervical cancer has greatly increased deaths of women, many of whom are young, with small children.
“The key for treating cervical cancer is discovering it as quickly as possible,” said Dr. Joseph Bernard Jr., the lead physician at Innovating Health International in Tabarre in metropolitan Port-au-Prince. The cancer treatment center provides low-cost chemotherapy to about 220 cancer patients a month.
“Patients come late,” he said, “not because they haven’t seen a doctor, but because doctors are not able to diagnose cancer on time.”
HIGH COSTS
Pelvic pain and bleeding were the symptoms that initially forced Paul to seek medical treatment earlier this year. After 12 days in a hospital near her home without a diagnosis, she went to Mirebalais. The lab tests, at $466, were unaffordable.
She sought out a private doctor in Port-au-Prince, who ordered up less expensive tests and told her the bad news: “I had cancer.”
He offered surgery. He did not offer radiation therapy, which is key to curing or controlling cervical cancer not treated by surgery. A treatment for more than 50 percent of cancers, radiation can kill off the bad cells and stop the disease’s spread.
But even surgery alone was more than she could afford, at about $1,500.
“I didn’t have it. I ran back to Mirebalais,” she said.
A doctor there told her that the cancer, though advanced, had not yet reached a non-treatable stage. A combination of chemotherapy and radiation, the doctor said, would give her the best chance at a longer life by shrinking the tumor and controlling the disease. But for radiation, Paul would have to go to the neighboring Dominican Republic, and it would cost $10,000 to $15,000.
“I told them I wasn’t going to the Dominican Republic because I don’t have money,” she said.
Her only option was comfort care, called palliative chemotherapy. “They said they will give me medication to ease my pain,” she said.
Dr. Ruth Damuse, the oncology program director at the Mirebalais hospital, said it’s not easy putting patients in palliative care when you know there is a treatment that could save them — but that treatment, radiation, is not in Haiti.
“They could be cured and they are not. It’s very difficult for me as a physician, and as a woman, and as a person in general,” she said.
In August, three days before her next scheduled session of palliative care, Paul scraped together the money. Her sister gave her $1.70, enough for a one-way motorcycle taxi ride to Mirebalais, and she figured she would plead her case to the hospital’s social worker, Oldine Deshommes, for help returning home and paying the $28 for her labs. She would have to sleep in the yard on a piece of cardboard for several nights during the tests and treatment.
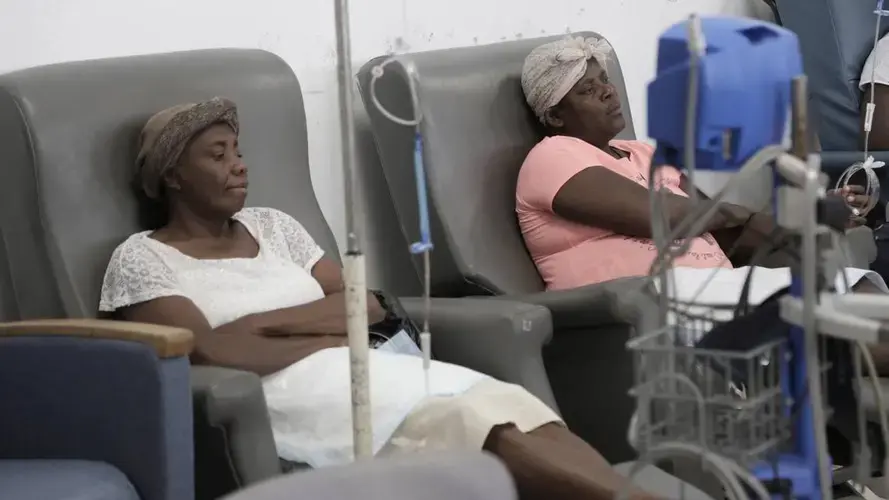
At the hospital, Paul found dozens of other patients too poor to pay for lodging all gathered in a covered breezeway — including her friend, Feonia Licin, 51, who’d lost her left breast in December to cancer. Licin was on her 24th day sleeping on the hospital grounds, stringing two chemo sessions together because she couldn’t afford the trip back and forth to her home 12 hours away.
On Paul’s third night, as a rainstorm pounded and water poured off the edges of the roof, she spied two wooden benches. She picked her way through the curled-up figures spread on the ground, and pulled the benches together to make a bed.
Though her own stomach ached with hunger, she was thinking of her children, Marie Stacey and her 21-year-old son, Kajilly, still at home. She had decided not to give up Marie Stacey to an orphanage, she said, even though she still didn’t have school fees.
Cancer had already stolen her role as the provider. She feared it would steal her daughter’s future, too.
“Every time she sees children going to school, she cries,” Paul said, tears welling. “I can’t let her not go to school again.”
The morning of her chemotherapy, Paul waited to turn in her test results to doctors who would decide if she could withstand the treatment. She was anxious, sitting one minute and standing the next, outside the Roselène Jean Bosquet Cancer Center, which opened in February. It’s named after the first patient that Partners In Health treated for cancer in Haiti — but even she had to go to the Dominican Republic for radiation.
And that free radiation program has ended now, due to lack of money.

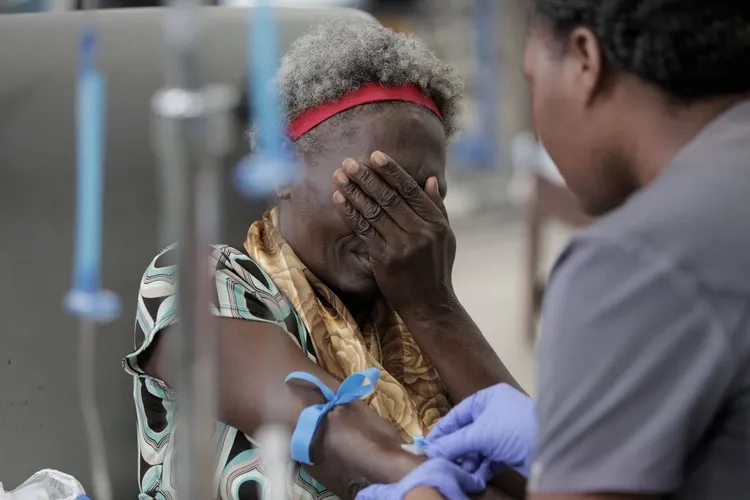
When her name was finally called at 9:33 a.m., Paul jumped up. Wearing a scarf on her head and a pink top with the words “That’s Life” scrawled across it in French, she walked into the crowded treatment room. A strike by the hospital’s support staff over raises had shut down the facility for two days. With 28 patients to treat, extra chairs were pulled in as saline bags were checked and chemotherapy prepared.
Just after 11 a.m., Paul finally sat down in a treatment recliner, with Licin in the chair next to her. She extended her left arm and covered her face with her hand. Three hours later, she took a bus back home to Bellanger, unsure whether she’d be able to return to the hospital for her next treatment.
RELYING ON GENEROSITY OF U.S. FAMILY
When Guerda Janvier was diagnosed with cervical cancer in 2015, she had a not-so-secret weapon — financial help from a network of friends and family.
“If I didn’t have money, I would have died already,” she said.
Initially, the cosmetologist, 46, was told by a doctor at the General Hospital that her cancer was operable, so she believed a cure was in the offing.
But surgery never came. Instead, a public health crisis paralyzed the hospital in 2016. Medical residents, upset over low pay and poor working conditions, went on a months-long strike.

Unable to get her surgery, Janvier traveled two hours by bus to Mirebalais, she said, where she was almost certain doctors at the modern facility, with its six operating rooms, would be able to help. The prognosis was not what she expected.
“The doctor looked at all of my exams, and said, ‘Madam, I can’t do anything for you. You might as well await your death,’” Janvier recalled.
She was devastated. “I started crying. I cried a lot,” she said.
Then she fought back, telling the doctor: “You don’t have a right to tell me to go take pills and await my death. You are not God. Only God can decide when I’m going to die.”
She found a different doctor, one who would operate. He even offered to charge half his normal fee of $1,400 by performing the surgery at another public hospital — once the strike ended.
So again, she waited. In the meantime, another tragedy struck. Her 21-year-old son was killed by a stray bullet on May 29 — Mother’s Day in Haiti. Janvier fell into a deep depression, unable to think about her own health for months. Eventually, with the help of a psychologist friend, she returned to the search for a doctor to operate.
That was two years ago. Now it’s been been three years since her diagnosis, and Janvier has seen so many doctors she’s lost count.
“I am seeing doctors. I am spending money. I am buying medications. The medications are wasting. They aren’t doing anything for me,” she said describing her fruitless search for a cure. “And yet a doctor said I was operable.”
In June, still looking, she ended up at Innovating Health International, the nonprofit in Port-au-Prince.
To pay for chemotherapy there — and for the doctors she has consulted — Janvier has relied on the generosity of friends and her husband’s elderly mother, who lives in Boston. She’s been too ill to continue working, so they’ve helped her come up with the 25,000 gourdes — about $358 — that Innovating Health International charges her for treatment that the doctors say could possibly shrink her tumor, making it possible to operate.
In neoadjuvant chemotherapy, as it’s called, chemo shrinks the tumor in preparation for surgery. Some studies have shown that when radiation treatment isn’t available, patients’ survival rates could be increased by the therapy.
Bernard, the physician treating Janvier, told her she may be able to get surgery, depending on how much the tumor shrinks. But the advanced stage of the cancer and issues with her kidneys raise questions about whether she is an ideal candidate for the operation.
Janvier has pinned her hopes on it anyway. “The way I used to care for my children, I can’t do it the same anymore,” she said, days later at her home in La Plaine, on the outskirts of the capital. “Once someone told me I could be operated on, it made me happy, because [before that] I didn’t have any hope of having surgery.”
‘NOBODY SHOULD DIE OF THIS DISEASE’
In the United States, cervical cancer rates have declined over the past 30 years because gynecologists have been able to identify and treat precancerous lesions — largely through Pap smears — before they develop into cancer. The HPV vaccine, given to girls and boys before they become sexually active to prevent cancer-causing infections, has also been available since 2006.
But in Haiti, those prevention measures are only just now gaining ground. And that means that “Haiti is among the countries with high incidence and mortality by cervical cancer,” said Laia Bruni, an epidemiologist and director of the Spain-based HPV Information Center of the Catalan Institute of Oncology, which serves as a clearinghouse for cervical cancer data.
Almost everyone who is sexually active will be exposed to HPV in their lifetime. In many cases, the body clears up the infection in one or two years. Although most cervical cancers are caused by HPV, most people who have contracted the virus do not develop cervical cancer. Men with the infection can develop head and neck cancers.

Left untreated, a precancerous lesion can take up to 10 years to become cancerous — if it ever does.
“It is a preventable epidemic,” emphasized Dr. David Walmer, an associate global health professor at Duke Global Health Institute, which has partnered with the Family Health Ministries medical nonprofit that he started to combat cervical cancer in Haiti. “Honestly, nobody should die of this disease.”
Walmer has been researching cervical cancer in Haiti for 25 years. Since 2014, his group has screened more than 23,000 women between Port-au-Prince and Leogane for HPV. Testing for the presence of HPV, he believes, is much more accurate than a Pap smear or visual inspection of the cervix.
Walmer says Haiti’s high cervical cancer rates have two primary causes: the country’s poor healthcare system and its culture.
“There isn’t an organized national healthcare effort to identify and treat precancer lesions,” he said. “Cervical cancer is also a little higher in Haiti because it is culturally acceptable for a man to not be monogamous after marriage, which increases the likelihood that he will spread HPV from one woman to another.”
Haitian women also are at risk due to poor nutrition and multiple pregnancies, other doctors assert, and gynecological visits are not part of many Haitian women’s medical routine. Pap smears are expensive, $25 or $30, and are available only in the country’s two largest cities, Port-au-Prince and Cap-Haïtien.
Bernard, the Innovating Health physician who became involved in cancer care three years ago, calls the frequency of cervical cancer in Haiti and its high death rate “a failure of our health system.”
But there seems to be little political will, which he and others say is needed, to invest in the healthcare system in Haiti.
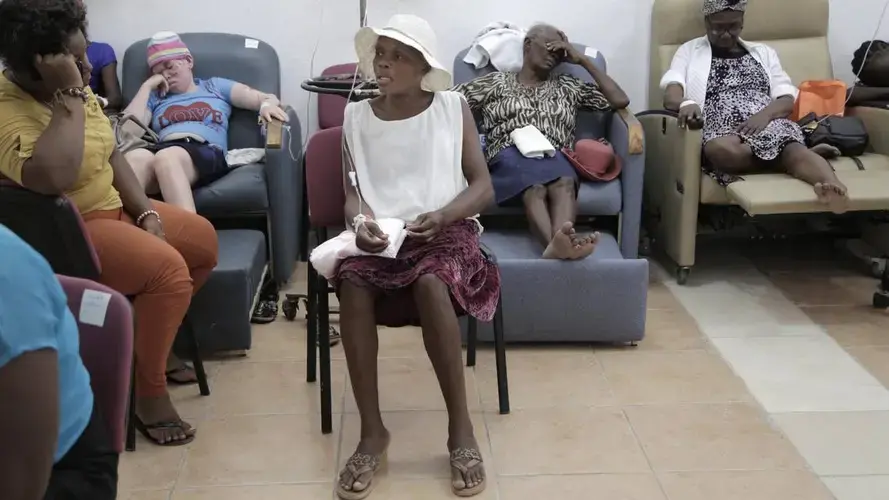
A 2015 World Bank report found that while Haiti has more hospitals per capita than some poor African countries, it spends less on healthcare per capita than its closest neighbors. The Dominican Republic spends $180; Cuba, $781; and the region of Latin America and Caribbean as a whole, $336. Haiti spends a rock-bottom $13.
A recent analysis of the country’s budgets over the past eight years by a Port-au-Prince economic think tank, Group Croissance, shows that the Haitian government spends more on its parliament and servicing its public debt, owed mostly to Venezuela, than on health. The debt service is more than twice the healthcare budget.
That doesn’t seem likely to change. In September, after committing to spend more on healthcare in the 2018-2019 budget year, parliament agreed to slash the health budget by more than half to just $86.2 million.
That means at the public General Hospital, where there are only four beds for chemo, patients have to pay for their own drugs to fight cancer.
It also means that with no financial assistance from the Haitian government for the poor streaming through their doors, nonprofits, their donors and doctors find themselves rationing healthcare: Which patients do you accept, and which do you turn away? Do you spend on rare lung cancers or save the money for more frequently seen cervical and breast cancers?
“You have to be very careful. You have to prioritize how you use your limited resources,” said Lori Buswell, executive director of the Center for Global Cancer Medicine at the Dana-Farber Cancer Institute in Boston, which provides almost $200,000 a year to Partners In Health for its cancer program in Haiti.
“With what you would spend to treat a single patient, you could potentially treat dozens of patients with what is available,” Buswell explained. “We need to focus on curing whatever patients we can and then looking at innovative ways to deliver care that wouldn’t necessarily be the same type that we would be able to deliver in a high-income country but do the best we can, given the resources.”
REVERSING THE TREND
But there is progress. Initiatives are under way to reverse Haiti’s deadly cervical cancer rates and create a national cancer screening program and a registry for tracking cancer.
“At the end of the day, if you’re able to see and treat more women, screen better, provide HPV testing and HPV vaccines, we will be able to say cervical cancer is part of the past and not the future of Haiti,” said Elizabeth Campa, senior health and policy adviser for Zanmi Lasante, which is Partners In Health’s sister organization in Haiti. “This is the new battle.”
Prevention, though, will come too late for Janvier, the woman who was told her cancer was probably operable. More than anything, she wants surgery so she can reclaim her life.

“Every time I think about it, I have palpitations,” she said. “I am always thinking. Some nights I don’t sleep because I have this sickness inside me.”
On her fourth visit to the clinic at Innovating Health International, where there are more patients than available recliners, Janvier tries to be upbeat. She has lost a lot of weight but jokes about it, calling her newly thin frame “sexy.” All of her hair is gone, and she, like Paul, thinks a lot about her youngest children, 11 year-old fraternal twin girls, Briana and Brithney.
“I love them a lot,” she said, her face lighting up for a moment. “I’m always saying, ‘God, I wouldn’t like to die and leave them’ because when I see how sick I am, it looks like I’m going to die.”

Image by José A. Iglesias. Haiti, 2018.
She’s impatient — and then worried.
“I would like to be done with the chemotherapy so I could have surgery,” Janvier said.. “Sometimes I ask myself, ‘Are they really going to operate on me? You think the hospital is really going to let me have the surgery?’ ”
Damuse, the Mirebalais physician who started a yearlong oncology fellowship at the University of Miami’s Sylvester Comprehensive Cancer Center in October, said doctors have to be careful not to oversell hope. She said there is no evidence that chemotherapy would help enough to allow a patient at Janvier’s advanced stage to get surgery as a treatment.
“To give [chemotherapy], we have to be sure that at the end, the patient will have surgery,” Damuse said.
As she holds out hope that surgery will end her cancer, Javier has struggled to answer one question — how she got this brutal disease in the first place.
“I asked myself, ‘Did I get it from some meat I ate? Or did I get it from having sexual relations with my husband?’ ” she said.
Not long ago, she confronted him. “I asked him, ‘Are you the one who gave me this cancer? Because they tell me if you had an outside woman, you could give it to me.’ ”
Her husband, Janvier said, told her that people who haven’t had sex yet still get cancer, so the disease wasn’t necessarily his fault. Unconvinced, she says she has refused to have sex with him until he seeks treatment.
But even though she now understands the cancer was caused by a virus, she still reverted to old-style Haitian mysticism while seeking a cure.
Janvier, who converted from Catholicism to Protestantism after she got sick, said relatives convinced her to take a six-hour bus trip to bring coffee and moonshine to the graves of dead family members as an offering. She got lost, she said, and never made it there.
Today, her faith is in God — and the possibility of surgery. That’s given her a new determination to beat cancer and prove wrong the doctor who told her to prepare for death.
After her August appointment, she missed two more chemotherapy appointments, though, because of poor kidney function. Her doctor, Bernard, says she may need to begin palliative care soon.
Janvier is undaunted.
“I am praying, I am asking God if he can help me find the money to operate,” she said.

Education Resource
Meet the Journalists: Jacqueline Charles and José Antonio Iglesias
"If people don't know that the problem exists, then how can you even begin to find a solution?"...






