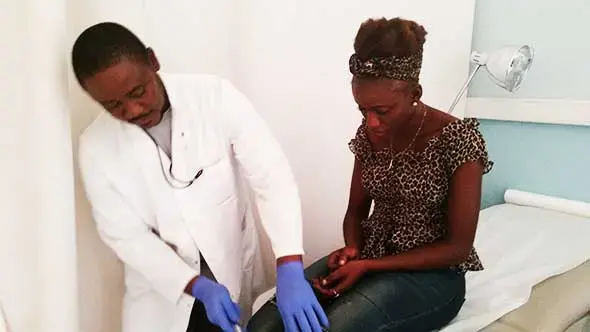
MONROVIA, Liberia—Josephine Karwah stepped out of the Ebola treatment unit and cradled her pregnant belly. She had hobbled into the white tent two weeks earlier, during August of 2014, her knees burning with pain and threatening to buckle every fourth step.
Josephine's mother had died in the Ebola treatment unit. Her body had been carried away in a white body bag that nurses had prepared with her name written neatly on the side. Her father, too, had died from Ebola, as did her aunt and uncle. But Josephine and her unborn child were survivors. She decided she would name the baby Miracle.
Then the nightmares began. Back at home in her village, Smell No Taste, an hour's drive east of the Liberian capital, Josephine dreamt of the family members she had lost to Ebola and the horrors of the treatment unit. Throbbing headaches interrupted her dreams and her hips and knees ached as she tried to fall back asleep. During the day she helped her older sister make soap to sell at the market. But her right eye burned and her left eye made the world appear cloudy, as if drops of dew had settled on a camera lens. At the money changer's booth, she walked away with the wrong change, unable to recall how many Liberian dollars were in her purse when she left the house.
Josephine is one of Liberia's 1,500 Ebola survivors. Like Josephine, many today suffer memory loss, joint pains, muscle aches and eye problems. These are not isolated anecdotes and vague reports. Just last week, reporting the first findings from the largest-ever study of Ebola survivors at a conference in Boston, Mosoka Fallah, an epidemiologist from Liberia, said more than half of the patients who lived through an acute attack later reported muscle and joint problems. Two thirds had neurological difficulties and 60 percent reported eye problems approximately one year after Ebola infection.
Doctors began referring to this constellation of symptoms as post-Ebola syndrome as early as fall 2014 when the World Health Organization sent a team of researchers to Sierra Leone. Half of the Ebola survivors they met reported eye problems, including blindness. And this has happened before. Following small Ebola outbreaks in east and central Africa in the last 20 years, survivors suffered joint pains, muscle aches and eye problems serious enough to prevent many from working.
But these were limited episodes of the disease and small groups of survivors. The 2014–16 west African Ebola epidemic has left 17,000 survivors at risk of post-Ebola syndrome. Like Josephine, they stepped out of treatment units and stepped into an uncertain future. There is one thing that experts and patients do know: Ebola is not over.
Ebola's Ghost
Fallah's office sits at one end of a long corridor in the John F. Kennedy Medical Center in Monrovia. A Harvard-trained epidemiologist, he grew up in one of Liberia's largest slums and was deep in the trenches as part of the Ebola response. Now he is at the helm of the largest-ever study of Ebola survivors. When Fallah talks about Ebola he often refers to the epidemic as a pitched battle and then quickly returns to more medical language. "At the height of the war, er, outbreak…" he says, researchers set in motion a project that led to his survivor research.
To test experimental vaccines and other treatments, a coalition was formed between the National Institutes of Health in the U.S. and the Liberian Ministry of Health and Social Welfare called the Partnership for Research on Ebola Vaccines in Liberia (PREVAIL).
By the time the initial vaccine safety tests were completed, however, Liberia's epidemic was slowing down. The number of people becoming infected with Ebola was far fewer than expected, so the first study, PREVAIL I, was scaled back to test only for vaccine safety and immune response and not the vaccine's ability to prevent Ebola. Instead, PREVAIL scientists shifted resources to Ebola's aftereffects. Reports were coming in from across west Africa of patients who survived the disease but suffered physical and psychological problems. That is when Fallah got involved. He was appointed principal investigator for the study in Liberia and switched his focus from the Ebola response to Ebola survivors.
On a Wednesday afternoon, two days before Christmas, Fallah flicked through a patient file at the Kennedy Medical Center. He had overseen the refurbishment of the building's second floor, which was now entirely dedicated to the Ebola survivor study. Outside his office and stretching up the corridor men and women sat in chairs that lined the walls waiting to be seen by medical staff.
Since the Ebola survivor study was launched in Liberia last June, more than a thousand of the country's 1,500 Ebola survivors have agreed to take part. Their health will be monitored at semiannual checkups for five years. Each survivor is asked to bring four friends or relatives to one of the study's three sites. These are people with whom the patients have close contact but who were not infected with Ebola. Fallah says he hopes to enroll 6,000 close contacts who will serve as controls, helping researchers separate the health problems that are part of post-Ebola syndrome from the those experienced by the general population in Liberia.
When Fallah presented the first findings from the study last week, he had grim numbers: 60 percent of the approximately 1,000 virus survivors in the study reported eye problems, 53 percent said they suffered muscle aches and joint pain and 68 percent reported neurological problems. When Fallah's team looked more closely at those who said they had eye problems, they found 10 percent had uveitis, a swelling of the middle layer of tissue in the eye wall. The eye problems drew his attention early in the research. "We saw as the war went on—I mean, the epidemic went on—that there were different manifestations among survivors and that would drive us to do more in-depth sub-studies," he says. Those secondary investigations are part of PREVAIL III.* "It was clear the first PREVAIL III sub-study had to focus on the eye."
Fallah looked to previous studies of Ebola survivors dating back to the 1990s and found that many described eye problems in the convalescent phase. Following an outbreak in the Democratic Republic of the Congo in 1995, 20 survivors were examined over three months. Four were found to have eye pain, sensitivity to light, loss of visual acuity and uveitis up to 10 weeks after infection. After an outbreak in Uganda in 2007, 49 survivors were followed for more than two years. As well as memory loss, joint pain, sleep disorders and hearing loss, survivors reported blurred vision and pain behind the eyes. More recently a study of eight patients who were treated for Ebola in U.S. hospitals found that all suffered various symptoms of post-Ebola syndrome up to four months after leaving the hospital. Six had psychological problems including depression, anxiety and memory loss, and five suffered eye problems including blurred vision and eye pain. There was no doubt the syndrome was real. But the existing data offered little explanation for how the virus can cause these problems.
Understanding the Damage
This kind of confusion has happened before, with another virus: HIV. Back in the 1980s when researchers were presented with this new health threat, they tried to understand this novel retrovirus by applying what they knew about other diseases. The same process is happening with Ebola, says Avindra Nath, a neurologist and scientist at the NIH who works closely with Fallah.
Nath has spent the better part of three decades studying infections of the brain. Although Ebola is not a retrovirus like HIV, Nath believes that years of research invested in studying HIV and the body's response to the infection have jump-started our understanding of how Ebola affects the nervous system. "Ebola has benefited from HIV research. A lot of us involved with Ebola made our careers with HIV so we are quickly adapting our knowledge and techniques to studying these patients," he says.
Nath wonders if the neurologic symptoms in Ebola survivors are a direct result of the virus or, instead, triggered by the immune system's response to the infection. HIV, for instance, infects immune cells called macrophages in the brain, prompting the release of cytokines, small proteins that are toxic to nerve cells. Studies in monkeys have shown Ebola also infects macrophages. Ebola also can trigger a massive "cytokine storm"—cytokines are chemical messengers between cells, highly active during an immune attack—causing veins to leak and burst. That can cause hemorrhaging throughout the body, including the brain, which could explain the memory problems, headaches and movement disorders Nath has seen in Ebola survivors during his visits to Liberia.
As the neurologist looks to HIV for clues to how Ebola affects the brain, others turn to different viruses to understand another symptom: the extreme fatigue in Ebola survivors. Studies have shown that up to a quarter of patients with the dengue fever virus and close to 40 percent of Epstein–Barr virus patients suffer fatigue after the acute illness. Inflammatory cytokines may be to blame. They can act on receptors in the brain causing post-infection fatigue and loss of appetite.
Painful joints seem to be one of the more common symptoms of post-Ebola syndrome. In a study of survivors of the 1995 Congo outbreak almost two thirds experienced joint pain two years after infection and one third of a Ugandan outbreak's survivors suffered from joint pain two years later.
Lumps of immune system proteins that sit inside a joint like the hip or shoulder could cause irritation and swelling. Other components of the immune system, including antibodies, could explain or even act as a surrogate marker for joint pain. After the 1995 Congo outbreak survivors who complained of painful joints were found to have higher antibody levels compared with survivors who did not report joint pain. Another protein might be at work in pain, too. D-dimers, small chunks of protein that break off from blood clots, have been linked to joint pain in people recovering from other infections. Patients suffering joint pain after infection with the bacteria Neisseria meningitidis had high levels of D-dimers in their blood. Studies looking for D-dimer–level changes have not been done on Ebola survivors.
Hiding Places
As for the eye disease seen in many Ebola survivors, experts say it too could be a result of the immune response to Ebola. Or, more ominously, the virus could be replicating in the eye long after it has been cleared from the blood. The eyeball offers a safe place for the virus to hide out, away from detection and interference by the immune system. In one survivor the eyeball was found teeming with Ebola. In October 2014 an American physician, Ian Crozier, fell sick with Ebola while working in Sierra Leone. Less than two months after he was discharged from a U.S. hospital he felt pain in his left eye and noticed that its color had changed from blue to green. When doctors inserted a needle into Crozier's eye, they found more copies of the virus than had been in his blood when he was close to death weeks earlier.
The eyeball is not the only hiding place for Ebola. The testes, central nervous system and joint cartilage can act as sanctuary sites for a number of pathogens including HIV. These vital structures are at risk of collateral damage when the immune system wages war on foreign invaders. So to protect themselves from the inflammatory response, they have adapted clever mechanisms including immune-suppressing molecules and physical barriers. These protective measures make them great hiding spots for viruses. Hidden reservoirs could explain how Pauline Cafferkey, a Scottish nurse who recovered from Ebola, fell sick nine months after her blood tested negative for the virus and again a year after she was first infected.
The testes could also account for why Ebola persists in the semen of some survivors months after they are free of symptoms. At the beginning of the west African outbreak, WHO cautioned people to practice safe sex for at least three months after their blood tested negative for Ebola. That advice was based on the 1995 Congo episode where the virus was found in the semen of survivors 82 days after symptom onset.
But during the west African epidemic, Ebola virus lived in the semen of some survivors for a much longer time, more than a year after acute infection. At the conference in Boston last week, Fallah reinforced these finding, saying the virus was found in the semen of Liberian Ebola survivors 18 months after infection. In some men the virus disappeared from the semen and then reappeared over the course of the year. (The WHO now advises male Ebola patients to practice safe sex for a year, and get their semen tested repeatedly.)
In his Monrovia office Fallah has a patient file that belongs to a woman whose son died of Ebola in November 2015. The family reported no contact with anyone sick with Ebola or any survivors, but Fallah believes otherwise. He thinks the mother may have had sex with a survivor, not realized that she was sick with Ebola and passed the infection to her son.
It would not be the first time Fallah had investigated a case of Ebola that was likely transmitted via sex. In March 2015 a woman who died from Ebola was found to have had sex with a man who had been discharged from an Ebola treatment unit six months earlier. Blood samples from the man tested negative for Ebola but a semen sample tested positive.
Fallah furrows his brow when talking about the woman who contracted Ebola from a survivor. That the virus can persist after many symptoms stop—even after a patient's blood appears clear-- makes him anxious for two reasons: If Ebola hides out in people who seem healthy, only to reappear from compartments deep within the body to make them sick and potentially contagious, it could spark more outbreaks.
But finding the viral genome or bits of viral RNA in the bodily fluids of survivors does not prove they are contagious, he adds. What really worries Fallah is the stigma these new findings place on survivors. "It's bad enough with post-Ebola syndrome that they have these symptoms we can't explain—and for who knows how long," he says. "Survivors are going through enough. Now imagine people are scared of them for fear of catching the virus."
Tragedy in the Womb
A few days after Josephine left the Ebola treatment unit in Monrovia, while she was sleeping in her bed in Smell No Taste, she woke just after midnight. This time it was not nightmares or headaches, it was cramping in her abdomen. She rose to use the bathroom, and when she wiped herself she saw blood on the tissue. Then her water broke. "Ophelia!" she called for her older sister. They phoned for an ambulance but were told none were available. So they called a radio station in Monrovia for help. No one came.
Josephine paced up and down her bedroom, stopping to press her palms against the wall when it felt like her stomach was tearing. At 5 A.M., she wrapped herself in a maroon lapa, a traditional Liberian saronglike fabric, and staggered out of the house. If help would not come to her, she would find help on the streets. The village was asleep, sunrise still an hour away. Josephine walked alongside her house, clutching the walls to steady herself. As she screamed, women came out of their houses. "Help me, please help me," she cried. But no one would come near her, fearful of touching the woman who had left the Ebola treatment unit only a few days ago. When she reached the light green house at the corner of the dirt road, Josephine could no longer walk. She fell to the ground, her back against the wall and felt the baby between her legs.
Five women approached, unwrapping their lapas as they walked. They formed a semicircle around her so the male onlookers could not watch her give birth. Josephine pushed and screamed and Miracle was born. What a chubby boy, she thought, lifting the silent child to her chest. But Miracle was not breathing.
No one would touch Josephine. The women stared as she rocked her baby and sobbed into her chest. Only her brother came close to her. He took Miracle from her arms and wrapped the baby and placenta in a yellow towel, ready for burial.
Josephine's mother had been a midwife before she died of Ebola. "Why isn't she here to help me now?" Josephine wondered. In the weeks that followed, there were more questions: Did Ebola kill Miracle or was it because nobody would help? Would the baby have lived if an ambulance had come? Was the virus still lurking in her body, and would it harm any future pregnancies?
On visits to the Kennedy Medical Center for her survivor study appointments, Josephine asks Fallah these same questions. One afternoon she sits in Fallah's office wearing an off-the-shoulder leopard print shirt and a matching head wrap waiting for his response.
Fallah worries the uterus may be another sanctuary site for Ebola, offering the virus a safe place to hide. Then he wonders if the stress of being an Ebola survivor can cause a woman to give birth to a stillborn baby in the street with people watching but no one helping. He thinks, "When you can no longer sell soap in the market, when you have to wrap your money in tissue to buy vegetables, when your boyfriend stops loving you because you are an Ebola survivor—What impact does that have on a person's body? What could that do to their unborn child?"
This is what goes through his mind, but when Josephine asks, he says: "I don't know, Josephine. We are trying to find out."
*Editor's Note (2/29/16): This sentence was edited after posting to remove an erroneous reference to one of the other PREVAIL studies.