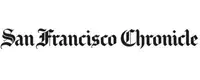A team of birth keepers in Washington is drawing on Indigenous knowledge and culturally competent care to help Native women reclaim birthing practices, parenting practices, and community. They’re also saving lives.
SEATTLE—It was the first year of the new millennium, and Abigail Echo Hawk was 19 years old, pregnant, and terrified.
The then-teen—a citizen of the Pawnee Nation of Oklahoma—followed her sister to Seattle, from where they grew up in Alaska, for medical care. She had her first appointment at one of the largest birthing hospitals in the city, what is now Swedish Medical Hospital.
A medical assistant, scanning Echo Hawk’s chart, asked if she was Native American.
“I said yes, and she automatically started treating me differently,” Echo Hawk remembers, two decades later. “She questioned me for about 10 minutes about how much I had been drinking, and then pulled back my sleeves to see if I had track marks from needles. I actually don't remember what happened afterwards, I was so traumatized by it.”

As a nonprofit journalism organization, we depend on your support to fund coverage of Indigenous issues and communities. Donate any amount today to become a Pulitzer Center Champion and receive exclusive benefits!
For two months, she avoided the medical system altogether. Then, in her second trimester, the teen sought treatment elsewhere, through the glass doors of the local Native clinic, the Seattle Indian Health Board. Twenty-one years later, Echo Hawk, now a mother of two, hasn’t left. She now leads the clinic as its executive vice president, and is also director of the Urban Indian Health Institute, where she advocates for state and federal policies to end racial bias in the medical world.
Echo Hawk’s experience from 2002 seems to be the rule, not the exception. Racial bias and discrimination in the American health-care system has proven disturbing at best and deadly at worst for pregnant Indigenous women, and it’s getting worse—not better.

Women in the U.S. already suffer the highest rate of maternal deaths—defined as death during pregnancy or up to a year afterward—among the world’s high-income countries. That chasm has grown greater since the 1980s. It has spiked dramatically in the past five consecutive years, according to federal Centers for Disease Control data.
Black and Indigenous communities bear the brunt of those maternal deaths: Native American and Alaska Native women in the United States are three times more likely to die during childbirth than their white counterparts.
It's even worse in Washington state, home to 29 federally recognized tribes. A report published in early 2023 by the state health department shows that Native mothers there die eight and a half times more often than white mothers during pregnancy or within a year after—more than any other race. That risk is equally shared among Indigenous women, regardless of income, education, or geographical location. Nationally, the CDC notes, that means that factors that typically reduce risk for white women don’t apply if you’re Black or Indigenous in America. The problem is racism, not race.
“Often what we're told as Native women is: We’re unhealthy. We're too addicted, too fat, too chronically ill, too poor,” said Camie Goldhammer, a Sisseton-Wahpeton tribal citizen and traditional birthworker in Seattle. “What that does is put the onus on the people who are dying. I really believe that moms and babies dying is the failing of our health-care system.”
More than 80% of all maternal deaths, the report found, were preventable. Although the problem is deeply rooted in systemic inequity for Black and Indigenous people in the United States, the solution is coming from the inside: In order to save Native mothers’ lives, Native mothers and aunties are taking on the cause themselves, by providing free physical, emotional, educational, and spiritual support to Indigenous mothers and their families before, during, and after their baby is born.
Since 2019, Goldhammer has developed a team of five Indigenous doulas, called Hummingbird Indigenous Family Services, who have provided culture-specific help to more than 150 Native pregnant women and their babies in the first thousand days of their baby’s life.
Their maternal and infant mortality rate has been zero.
The preparation
The word ‘doula’ is a Western name for what Indigenous peoples have always done—care for their mothers, said Echo Hawk.
Although Goldhammer and her team use the term interchangeably with ‘Indigenous birthkeeper’ for mainstream recognition, she explains her profession as “fulfilling the traditional role of an auntie,” by drawing upon Indigenous knowledge and experience to care for birthing mothers and, eventually, their babies.
“We became doulas because we were sisters and aunties and cousins who would attend the births of our sisters and aunties and cousins,” Goldhammer said. “As you do more of those, you learn more, like, ‘Oh, when the baby was breech, auntie did this for her.’”

Doulas are non-clinical, trained health-care workers who support pregnant women before, during, and after pregnancy. Their work is based around building a relationship with expecting mothers and their families from the time of pregnancy through the first six months of their child’s life. During that time, doulas help their clients write a birth plan, educate them on labor positions, are often present as an advocate during birth, and provide physical, mental, and emotional support. Unlike midwives, there is no state-level legislation requiring certification for doulas, though there are national certifying boards.
While nurses and physicians manage time during a woman’s labor and birth, “doulas and midwives help people move through time during labor and birth—and that’s a different skill set,” explained Monica McLemore, a scholar in antiracist birthing care and a professor of nursing at the University of Washington. “It’s a different model of care that I think is more humane [and] has better evidenced-based outcomes.”
Separately, a resurgence of Indigenous midwifery across the United States, Mexico, Canada, and New Zealand has brought birthing centers and Indigenous midwives back to the communities where they were once outlawed under colonization. Indigenous midwives are medical providers who can deliver babies, provide postpartum medical care to mothers and their newborns, and administer traditional medicines.
Doula-assisted mothers are four times less likely to have a low-birth-weight baby, two times less likely to experience a birth complication involving themselves or their baby, and significantly more likely to initiate breastfeeding, according to a 2013 study published in the Journal of Perinatal Education. “Communication with and encouragement from a doula throughout the pregnancy may have increased the mother’s self-efficacy regarding her ability to impact her own pregnancy outcome,” the study says.
The effectiveness of doulas is so convincing that numerous states—including, this year, Washington, after efforts from Indigenous advocates—have passed bills to expand Medicaid coverage to include doula care. As of 2022, more than half of all states are either providing such coverage, in the process of implementing it, or taking some related action to expand access to doulas statewide, according to the National Health Law Program’s Doula Medicaid Project.
For Indigenous people, having culturally competent care throughout the entire pregnancy, birth, and postpartum period goes even further. By intimately understanding the community they serve, Indigenous doulas are able to build trusting relationships with clients that assuages the buildup of toxic stress. That can lessen maternal morbidity, maternal mortality, and infant mortality.


Shannon Kopelva (a citizen of the Fort McDermitt Paiute-Shosone, Hualapai, and Hopi Nations from Moenkopi, Arizona) has always sought out medical providers of color, and it was no different when she learned she was pregnant with her first child. She wanted more support than infrequent prenatal checkups, and she also wanted to bring her child into the world with a sense of his Indigenous identity.
In late April, Kopelva was 38 weeks pregnant when her Hummingbird doula, T’leeuh Antone (they/them, a citizen of the Akimel O'odham Nation), pulled up to her house in downtown Seattle for their weekly visit.
Antone brought muslin wraps and a realistic brown baby doll to practice swaddling. Also in their car trunk was a traditional cradleboard for baby, as they call the unborn child, and materials to make medicine bundles of cedar herbs for the birth.
Seated around Kopelva’s kitchen table, Antone went over the birth plan Kopelva and her husband, Andy, could expect at the scheduled Cesarean section for her breech baby the following week. She was still hoping the baby would flip—Antone has been helping with natural positions to right breech babies in utero—so she could deliver naturally.
Since the 1970s, birthing has become a business in the United States. From the early ’90s through the turn of the century, births resulting from induction in the United States doubled—and about half of them for no medical reason. Today, Cesarean deliveries account for more than 30% of all births, and doctors and hospitals are generally paid more for them. The average Cesarean section costs $26,280, with $3,214 paid for by the individual, compared to an average cost for vaginal birth of $14,768 with $2,655 out of pocket, according to a 2022 analysis by the Peterson-KFF Health System Tracker.
“Short answer is: Surgical birth has always been perversely incentivized, because hospitals got more money for those,” McLemore said.
Kopelva’s birth plan included filling the operating room with Hopi music, traditional storytelling, and medicinal massage oils. “That’s what I need to capture, the smell of rain in Tucson,” she said, as busy hands wrapped cedar into small bundles to bring to the hospital.
“When the setting isn’t home, we’re trying every sensory way to bring culture into the space,” Antone says.

“I see a lot of this work is things that I would do for my family,” Antone says. When Antone’s mother gave birth to their younger brother two decades ago, a nine-year-old Antone stayed by their mother’s bedside through the birth. “It's all things that we intuitively did in our culture. So it feels very natural and loving to be able to be a support [in] reclaiming birth practices, parenting practices, and community.”
From Kopelva’s perspective, she likes that she doesn’t have to explain herself to Antone, and that they both share a “reverence for the desert.”
“It's really important and really great that it can be someone who understands where you come from and understands the customs, even if they [have different tribal customs]. You don't have to explain things,” she said. After the birth, she observed a traditional Hopi practice of secluding herself and her baby for 20 days indoors, before introducing him to the sun.
Afterwards, the new parents planned to travel to Arizona for their son’s traditional naming ceremony. “That's probably the biggest thing: not having to explain, and having that general understanding of what we do as Native people, and having that respect.”
The push
Indigenous birthkeepers fill the gaps Native women are falling through in the Western health-care system, in both the type of care they provide and when they provide it.
While many women don't meet their delivery doctor until they’re delivering, doulas build trusted relationships with their clients, and provide continuous care through the entire pregnancy, birth, and postpartum experience. They have the specialized knowledge and experience to help facilitate conversations between their client and provider, and often help advocate for their client.
That advocacy can be life-saving.
Alana Harris (Ojibwe), 28, wanted her son’s first scent out of the womb to be of sweetgrass. So for his birth in early July 2023 at Swedish Hill Medical Hospital, she tied a braid of sweetgrass—“a soft scent that makes you feel like home”—around her neck, and stuck another in the bassinet that would hold him. Then, she prepared to give birth.

Harris, who moved to Seattle at the end of 2020 from Chicago, had an easy pregnancy. Her blood pressure never spiked, she made every prenatal appointment, and she was vigilant about monitoring for the gestational diabetes her mother suffered from when she was in utero. She enrolled in Hummingbird’s doula program, and had weekly visits from her doula, Kristin Lightfeather (Comanche, Ojibwe), who helped guide her through what to expect in her birth. Particularly, Harris said, Lightfeather helped her envision how she wanted her birth to go—both mentally and spiritually.
“I was really blessed to have a very easy pregnancy,” Harris says, four weeks postpartum. “I had a go-to plan or thought process, which helped with anxiety big time. All signs pointed to: Everything should have been fine.”
Which is why it was so shocking when it wasn’t.
Harris went into the hospital on a Friday night for an induction at 42 weeks, per her doctor’s recommendation. Her plan was to deliver vaginally, pending any emergency or risk to the baby. Lightfeather was there, as was Harris’ husband Bear (Lakota), and a friend.
Throughout that Saturday, she began what would be the next 48 hours of dilation and pushing, with doctors periodically coming in to check on her. Lightfeather and Harris’ husband alternated massaging her pressure points to relieve the pain and help the baby drop for delivery.
Harris said it gave her confidence to know there was a professional there who she could turn to and be heard, and who already knew her wishes for her birth. “Not a lot of vocalization needed to happen,” Harris said afterwards. “I just looked at [Lightfeather] and she was like ‘yup, you're in pain’ and started certain alleviation methods.”
On Saturday evening, a care team of nurses prescribed Harris pitocin, a drug used to accelerate labor, after her dilation stalled at five centimeters.
Lightfeather realized things weren’t going according to plan when she overheard the number 30. She knows pitocin levels shouldn’t exceed 20 in a normal delivery because higher levels can cause fluid retention and even uterine rupture from hyperstimulation.


“So I spoke up,” Lightfeather said. Advocacy in clinical settings is an important aspect of her job as an Indigenous doula. “I was like, ‘Oh, wow. That's really high. It's supposed to be no higher than 20, correct?’ And the nurse kind of just turned around and walked over towards her computer, hollering over her shoulder towards me, saying ‘We can actually technically go to 40.’”
At every other birth she’s been to after four years as an Indigenous birthkeeper, Lightfeather said she’s worked in partnership with the clinical team to care for their client, not against them. She’s spoken up before: When she saw nurses roll their eyes at her client, she quickly dismissed them for a new care team. But at Harris’ birth, she was dismissed by the team of nurses and the doctor who would come in every few hours to check on Harris’ progress.
“I'm trying not to allow gaslighting behavior towards us [Indigenous birthkeepers] when we're supposed to be partners for these women,” Lightfeather said. “This can’t be the new normal.”
Harris had dilated to nine centimeters when her organs seized up from the pitocin, and she stopped urinating completely. Her legs filled with fluid. She began to feel a sharp pain in her right kidney despite the numbing effects of her epidural anesthetic, and when she told the nurse, she was offered a pillow to put under her. She developed pre-eclampsia, or a hypertension condition that can be caused by pitocin.
On Sunday, Harris’ Indigenous doctor from the Seattle Indian Health Board—the health clinic partners with Swedish for labor and delivery—who hadn't been on call when she went into labor, came into her delivery room. Harris had not urinated or dilated for 24 hours. The doctor immediately requested a second opinion from an obstetric surgeon.
The surgeon did an ultrasound, checked Harris’ vital signs, and said: “This baby should have been born ten to twenty hours ago.”
The baby weighed 12.5 pounds, and was delivered by emergency C-section on Sunday night. Harris lost two liters of blood during the delivery. Postpartum hemorrhaging, one of the leading causes of maternal deaths in Native women, can be caused by prolonged pitocin or high levels of pitocin, according to the American Journal of Obstetrics & Gynecology.
“There were so many points that [the nurses] should have gone and got a doctor, but the nurses were just like, ‘oh the textbook says…’” Harris told me, four weeks postpartum. “They just felt like it was all so routine. And it's like, people still die during childbirth. There's no routine to this.”
Although Harris and her son, Makoniibin—meaning summer bear in Ojibwe—are both healthy and recovering, Goldhammer’s team classifies the birth as a “near miss,” a reality that Harris is only just beginning to process.
Emotional support is a huge part of Lightfeather’s postpartum care for her—and of all Indigenous doulas for their clients.
“In the beginning, it was the feeling of: ‘I'm good. I'm okay. My baby is here,’” Lightfeather said of her client. “Then it went to the realm of: Why? How come it happened this way? And then it was: what if? What if this didn't happen? We had to do a lot of reflection together towards emotional healing.”
The recovery
Most maternal deaths don’t happen during delivery, but afterwards: 60% occur within a year after the birth, CDC data shows. Among pregnancy-related deaths for which an underlying cause was identified, the most common was mental-health conditions (suicide and overdose), which contributed to close to 20% of deaths. This surpassed hemorrhaging, cardiac and coronary conditions, and infection, and points to a very specific need for postpartum support that most women aren’t receiving.

Camie Goldhammer—whose shield of hair swings over her shoulder when she picks up her client’s teetering two year old—is an activist by all standards. Before she started Hummingbird Indigenous Family Services, she served as an Indigenous social worker who specialized in the effects of intergenerational trauma on attachment, bonding and parenting practices in the Native community. She has been a fierce advocate for breastfeeding as food sovereignty for nearly two decades, and ran an informal lactation group out of her Seattle living room for seven years before Covid hit. Still, Goldhammer travels across Indian Country for her second business as an Indigenous lactation consultant, where she and her colleague, Kimberly Moore-Salas (Diné) train Native people as breastfeeding peer counselors, or “Indigi-LCs.” To date, they have trained over 550.
From Alaska to South Dakota and beyond, she says, “almost everyone is traumatized from their birth. That is: You didn't die, but you were fucked up. You leave your birth broken. How does that impact your ability to freely love and attach to your child?”

But with support that mirrors traditional child-rearing practices—where Indigenous parents’ role was solely to love their child; it was the community’s job to help parent them—Goldhammer is striving to bring about intergenerational healing.
“That is the essence of reproductive justice,” she says. “It's not just the right to have a baby if you want to or not have a baby if you want to, but it’s also about the right to parent your baby in a safe and supportive environment.” In July, Hummingbird began a guaranteed basic income program to help reduce the burden of stress on Native families and improve health outcomes. Over the next five years, they will give up to 150 Indigenous pregnant women no-strings-attached payments of $1,250 a month, until their child’s third birthday.
Suicide and drug overdose are the leading cause of maternal deaths among Native mothers, the Washington health department report notes. Thirty percent of those deaths occur within 42 days after labor, which overlaps with a life-sized crack: Most obstetricians and primary-care doctors don’t see new mothers and babies for follow-ups until 42 days after birth.

Shanda Spencer (Diné) is a mother of three. After she gave birth to her third baby in April, her typical spitfire personality was replaced by something more sinister. She felt depressed—like her life was over—and overwhelmed with responsibility to her children, her boyfriend, and her home.
“I felt helpless,” Spencer said, one month postpartum. “My baby's crying, I had a C-section, I couldn't move around too much. With my other two children crying, I felt like I didn’t have a breather.”
When T’leeuh Antone, Spencer’s doula, showed up postpartum with her requested meal of BBQ ribs and spent a solid four hours with her, Spencer describes it as feeling like she could finally breathe and be herself again.
In addition to adjusting to a newborn baby, Spencer said she was missing her Native community back home in Arizona. She felt that kind of community with Antone.
“It was a sense of relief,” Spencer said, her eyes glancing at Antone rocking her sleeping baby nearby. “It felt like: my people are here. I can do this.”
- View this story on Elle