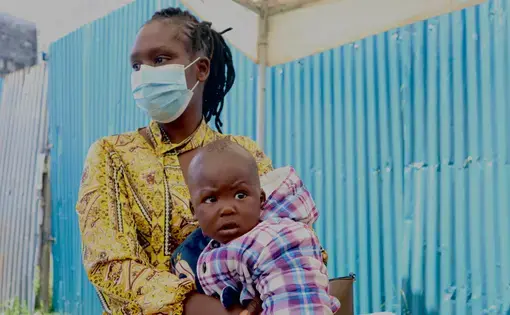
In five years, a Kenyan county with one of the highest maternal mortality numbers nationwide has changed its fortunes.
NANDI, Kenya — In 2005 when Kenyan authorities first told Jane Bett to stop assisting women with home births, the traditional birth assistant had mixed feelings. Helping deliver babies was her passion –something she had volunteered to do despite being a farmer primarily –but she had also seen tragedies happen when things went wrong.
“I saw a lot of women dying in my village. Women would lose a lot of blood, or their wounds were not tied up properly,” said Bett. “Sometimes you would try to help a mother but her placenta would refuse to come out and all you could do was pray. It was so dangerous.”
In 19 years, she helped deliver 40 babies in Koiban, her village in Kenya’s Nandi County – home to an estimated 886,000 people.
Almost a fifth of women across 11 countries in East Africa still prefer home delivery, according to a 2022 report by Ethiopian researchers. These births, usually with the help of traditional birth attendants and no health care professional present are mostly done under unsanitary conditions leading to high maternal mortality rates in the past.
In the last decade, hundreds of former midwives, so often evangelists of home births, have transitioned to educating expectant mothers on the importance of giving birth in proper healthcare facilities.
In 2013, Bett became one of them.
These days, she even accompanies pregnant women in labour as they race to get to the hospital in time, on motorcycles.

Community health strategy
The transition is being facilitated by Kenya’s Community Health Strategy. In 2000, the Kenyan government launched the programme to improve public health by training trusted local community leaders to become community health volunteers. It was initially piloted in a few counties before eventually spreading nationwide.
Volunteers spend about two hours per day educating their peers about primary healthcare. Many do this for free but sometimes they get stipends of up to 8,000 Kenyan shillings or $66 per month.
In Nandi County, that strategy seems to be working fine.
The percentage of women giving birth in the presence of a skilled birth attendant has almost doubled, from 37 percent in 2017 to 69.5 percent in 2021, according to the Kenya Health Information System (KHIS).
That is slightly better than the national average, which was 65.3 percent as of June 2021, according to KHIS.
It is a leap from 2009 when Nandi had the sixth-highest number of maternal deaths annually among Kenya’s 47 counties, according to a situation analysis by UNFPA, the United Nations sexual and reproductive health agency, using data from Kenya’s 2009 census.
Community health volunteers also make door-to-door visits to expectant mothers.
“We have the names and locations of all the pregnant women living throughout each sub-county,” explains Hellen Murei, a head nurse at a maternal health clinic in Nandi. “If a woman does not show up to her scheduled doctor’s appointment, we will try to call her phone. If we cannot reach her by phone, we will then contact her village chief, who knows where all the residents of his village live, and he will help us make a door-to-door visit.”
The volunteer programme is effective and also low-cost, making it feasible for many local governments to fund without international aid, according to Faith Onyangore, a lecturer and public health nutrition specialist at the University of Kabianga.
“The door-to-door methods … is a very sustainable approach,” Onyangore said. “In my own experience, I’ve seen places that did not have any international partners implement this programme and see it thrive.”
But the community health strategy was not always this efficient. Experts say Nandi’s success can be mostly traced back to a fundamental restructuring of Kenya’s government that took place in 2010.
Devolution and growth
In 2010, Kenyans voted for a new constitution that devolved power from the centre and among other things, changed the way resources were allocated to local governments.
Prior to that, Kenya was divided into eight legislative provinces with regional governments, each home to diverse ethnic groups. This was restructured into 47 counties with each having its own governor, health department, finance department, and more.
Many who work in community health care say that process has been key to some of the country’s improvements in the last 10 years.
“Before … community health strategy was being run by the national government throughout the whole country and the growth was very slow,” John Wanyungu, the health ministry’s deputy head of community health services told Al Jazeera. “But since devolution when counties were empowered to manage their own community health programmes, we’ve seen an exponential growth in community health units.”
According to Wanyungu, counties now tailor the healthcare funding they receive to focus on their specific needs at any point in time.
For Nandi, where incentivising women to give birth in hospitals was a top priority, devolution meant that local government was able to spend more of its resources on growing the community health volunteers programme and building more healthcare facilities.
Linda Mama
One more factor explains how Nandi County has reduced its maternal deaths: Linda Mama.
It is a universal healthcare coverage system for pregnant women in Kenya that launched in 2018. Linda Mama means “protect mama” in Swahili and the programme covers cost of delivery and routine check-ups for pregnant women nationwide.
“I gave birth at home to my first baby in 2012 because I could not afford it,” said Meryline Jepkemboi, a Nandi County resident.
She recently gave birth to her second baby in the hospital and says both experiences were markedly different.
“When you give birth in the hospital it is not scary. I was scared for my life the first time I gave birth,” Jepkemboi said. “I am so grateful for Linda Mama.”
Expecting reforms
Now that most women in Kenya are giving birth in the hospital, healthcare strategists are shifting focus towards improving the quality of care and data collection, according to Dan Okoro, an adviser at UNFPA.
“Over 80 percent of maternal deaths in Kenya today are due to sub-optimal care,” says Okoro. “This can include anything from a lack of proper equipment, supplies, or skills to disrespectful treatment of patients.”
Okoro also wants to see better data collection throughout the country. Over the last 10 years, data collected by the Kenya Health Information System (KHIS) has increasingly become reliable but data collected from the civil registration system does not often align.
This is due to several factors.
For one, many counties in Kenya including Nandi, do not track deaths during home delivery on an annual basis. Instead, maternal death is tracked through the Kenyan Population and Housing Census, which provides estimates for maternal mortality using birth and death certificates.
This survey is only published once every 10 years, and the most recent report uses data from the year 2019. Data for other years is usually extrapolated from mathematical models.
Streamlining the process to have uniform and reliable data systems would greatly improve the country’s ability to undertake evidence-based interventions, says Okoro.
While campaigning for the presidency, William Ruto, elected in August, pledged to reform the national health insurance fund platform and improve KHIS. If he delivers on his promise, it would be a game changer for maternal health in Kenya, Okoro said.
Back in Koiban, Bett is hoping for more intervention from the centre too. “We pray to God and hope that this new government will do something,” she said.