Part I of a IV Part Series
In 2020, the pandemic claimed the lives of my father, my youngest aunt, a disabled first cousin, and 14 other friends and acquaintances. They were among the 577,000 Americans who lost their lives in a span of 14 months, just a smattering among the 32.5 million Americans who reported being infected.
As the year crept to a close, I was grateful I had not contracted the disease. But before I could crack a bottle of champagne to ring in the new year, 2020 hit me with a sucker punch. By the time I regained control, I was tethered to a machine three times a week having been misdiagnosed with End-Stage Kidney Disease (ESKD).
Were it not for a bizarre, medical malfunction that nearly cost my life, I would have never known I didn’t need dialysis at all. What I really had experienced was Acute Kidney Injury (AKI), rapid loss of kidney function brought on by COVID-19. A report from the National Kidney Foundation (NKF) shows that people hospitalized with COVID-19 are at significant risk of AKI, which can lead to serious illness, dialysis, and even death.
The report also acknowledged there had been reports of nonelderly adults infected with COVID-19 who have developed an acute kidney injury (AKI) — sudden loss of kidney function. These adults did not have underlying medical conditions. With proper treatment, including dialysis in severe cases, AKI can be reversible.
NKF researchers explained further: “Kidney failure develops rapidly over a few hours or a few days,” the foundation warned. “…Patients hospitalized with COVID-19…, were twice as likely to develop AKI as compared to non-COVID patients who developed AKI during the same time period in 2019 – 56.9 percent versus 25.1 percent, respectively,” they said.

I spent months contemplating my own mortality, as I struggled to comprehend what was happening to my body. With the virus long gone, I now had to contend with the side effects of dialysis treatment, while trying to navigate the complex labyrinth of renal care. For the rest of my life, I believed I’d require 12 hours of blood purifying treatments if I intended to live.
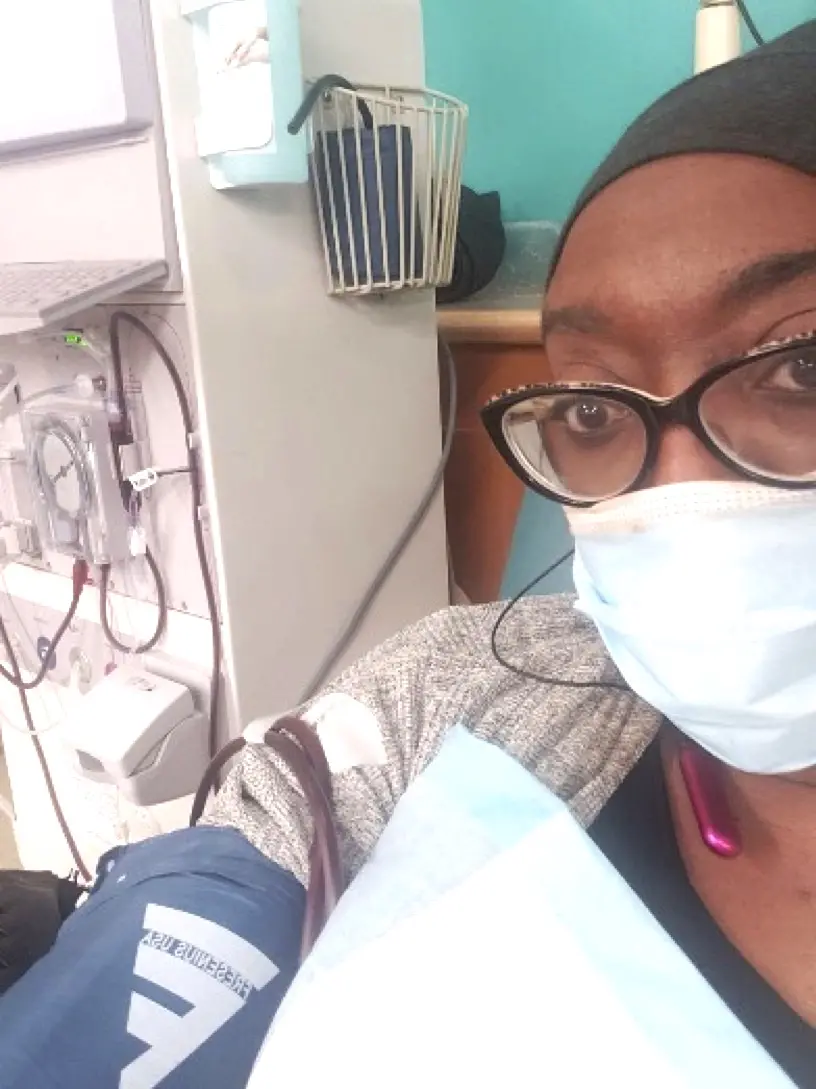
Assigned to Fresenius South Shore, I began treatments there just before Christmas. Less than eight weeks later, my chest catheter exploded with only 20 minutes left on the machine, and the staff called emergency while others held their hands to my chest trying to keep the blood from spilling out. The fire department arrived at the facility, assisted in stopping the hemorrhage. Then they carted me four blocks away to South Shore Hospital’s emergency room.
Had it not been for a previous bad experience there, I might have stayed and allowed the team to stabilize my wound and schedule me for surgery to insert another catheter. Instead, my instincts, sometimes called ‘mother wit,’ told me to leave. When I noticed the ER was unattended I took my bloodied self home, changed clothes, and went to Northwestern Hospital.
That’s what spared my life. It was a Friday. By the time I got to Northwestern, the surgery team that would have decided to give me a new device was gone. I’d have to be admitted for the weekend. After three days, a group of doctors and medical students trotted into my room with exciting news: I did not need to be on dialysis at all. I didn’t have end-stage anything, what I experienced was AKI. High five, Leak Funeral Home would have to wait. Though they remained baffled as to how or why the catheter exploded, one physician assured me it had been a blessing in disguise.
My family and I were joyful. Prayers had been answered. The experience left me frightened, angry, baffled, and yet determined to find answers to a multitude of cascading questions.
Chief among them was how could this have happened? How many people had that happened to? Were there others put on permanent dialysis when the treatment should have been temporary, at best? Has anyone died because of it? How would anyone know?
It seemed that nearly every mortality reported last year was a result of coronavirus or homicide—though in some of those cases the pandemic was still cited. Even suicides were being described as related to the pandemic. It was as if no one had died of cancer, heart disease, old age or any other malady. It was as if all other diseases had been put on pause.
The more I reflected on what I went through the more curious I became. Journalists are inquisitive and skeptical by nature. As writers, we see the world as it is, its beauty, its ugliness.
Beyond patient care, who else benefits from the dialysis business? What’s the success rate? Why was I called a customer and not a patient? Was that why I rarely had personal time with a doctor while under their “care.” Given, African Americans die at a higher rate of kidney disease, I started wondering who owns these dialysis centers in my community? They pop up like McDonald’s restaurants—and in some neighborhoods, they are the only new business ventures for blocks. Most of them are owned by Fresenius Medical Care of North America (FMC), DaVita Kidney Care, U.S. Renal Care, American Renal Associates and Dialysis Clinic Inc.
When former President Donald Trump authorized federal relief funds, over $250 million went to dialysis providers, according to government records examined by the Crusader. Of that, FMC, headquartered in Germany, received $137 million or more than half despite admitting it had ample financial resources, according to a Kaiser Family Foundation report.
However, in a Security Exchange Commission filing last July, the publicly traded Fresenius revealed it had, in fact, received a total of $277 million in taxpayer relief funds under the Coronavirus Aid, Relief and Economic Security (CARES) Act. In 2020, FMC earned $21.4 billion in revenue.
Its top competitor, DaVita, headquartered in Denver, initially accepted a $240 million bailout, but according to news reports at the time, returned the money citing a preference for the money to go to agencies that needed it most. DaVita reported earning an estimated $11 billion in 2019.
“From our perspective, they were a safety net,” DaVita CEO Javier Rodriquez said at the time. “And they were to be used for people that needed that money, because the economic damage was so severe, that they couldn’t keep their doors open.”
It is difficult and triggering for me to relive this experience, even through words. Recently, I chalked up my four-month ordeal as a foray into the “Twilight Zone,” a sort of alternative reality where weird stuff happens.
I could not help but wonder what might have happened to me if I had not been my own best advocate. But the bigger question I faced, like so many of my heroes and heroines before me, was not what might have happened to me. I also wanted to know who would look out for the lives of my neighbors.
For several weeks I sat side-by-side in a crowded dialysis center, among young and old, trying to live. Though I spent most of my four-hour treatment reading and writing, at times I enjoyed listening to the stories and tall tales of the elders who kept the place lively and not feeling like a pit stop before death.

I wondered if any of them had AKI and were in those seats because of COVID? Could any of them come off dialysis too? I was ticked off that the doctor on staff at FMC South Shore never contacted me when the catheter exploded. Once I got home, I called the staff nurse to let her know I was very much alive, and if she didn’t mind thanking the staff who assisted in ensuring I did not bleed to death. I also asked her to at least tell the other patients I was well—and that I didn’t need dialysis any longer.
When Dorothy R. Leavell, publisher of the Crusader, learned what happened, she encouraged me to tell my story. It was a debt owed for the blessing that had just been bestowed upon me. I admitted, however, that if I told the truth about my experience, that some people in my neighborhood might think I was attacking the only hospital we had.
As a longtime activist and strategist, no one has to tell me about the wanton “lack” that proliferates every aspect of Black lives. As part of a coalition of entrepreneurs, activists, artists, educators, and thought leaders working for a stronger South Shore, I was concerned that if I shared my experience publicly my efforts would be used to further destroy rather than build the community’s health care ecosystem.
Dr. King once said something about silence and complicity. If you witness injustice you must counter it with justice. Closed mouths don’t get fed and if no one knows there might be a problem, who will solve it?
I don’t wish what happened to me on anybody or any living being. Ironically, during my first dialysis treatment at a FMC clinic, I went temporarily blind and nearly died. The hemodialysis machine was set too high, causing my blood pressure to rapidly drop. “They got me coming in and got me going out,” I joked, not too long ago. None of my children thought that was funny.
The truth was neither did I. Now living with kidney damage (thanks COVID!) As I remain on a road of recovery and renewal, I am grateful for all of the people who put their lives on the line during the pandemic in service to others. Despite their own fears, they did their jobs and took many actions that saved many lives.
As I regained my health, I wondered if I would have shown up to work knowing every single day I was putting my life at risk by caring for people with an incurable, infectious disease. A lot of people bailed on employers, leaving hospitals, urgent care, and similar facilities understaffed and struggling to keep up with demands.
One Certified Nursing Assistant (CNA) told me she didn’t have a choice. “I need the money,” she told me. Her eyes were large, magnified slightly by the plastic face covering she wore. “I need my job.”
WINTER WAS COMING
By the time Winter 2020 rolled around, downtown Chicago looked like one of those abandoned towns in a Clint Eastwood western. All that was missing from State Street’s sparse traffic were tumbleweeds. The eerie quiet of a gigantic and vibrant city was a sobering reality of a pandemic.
Coronavirus disease (COVID-19) was declared a pandemic by the World Health Organization on March 11, 2020. Prior to this designation, it had been declared as an epidemic in mainland China near Wuhan in December 2019. The first case was reported in the U.S. in January of 2020 when a 35-year-old man from Snohomish, Washington turned up in an emergency room with a severe cough and fever. He told doctors his symptoms began four days after returning from China.
Black America, especially, was still reeling from the sudden death of NBA legend Kobe Bryant. Few had time to shift their focus to a mysterious, invisible disease, that the nation’s own president downplayed. “We have it totally under control,” Trump said at the time. “It’s one person coming from China, and we have it under control. It’s going to be just fine.”
Like most people, I followed all of the rules and mandates imposed by local officials anyway. I wore masks in public, I isolated and had no personal visitors. As the daughter of a nurse and something short of a germaphobe, I practice good hygiene and environmental cleanliness as a way of life.
For over 10 months, I’d been religious in keeping my immune system strong by eating vitamin-rich foods, drinking plenty of water, and taking brisk walks when I could. In decent health, there were times I wondered if the confusion in response to the pandemic was worse than the infection itself.
I found out the hard way that wasn’t the case.
Mayor Lori Lightfoot had emerged as something of a national folk hero due to her creative initiatives to keep Chicagoans safe. Through her “Stay Home Save Lives” campaigns, the city banned public events, shuttered parks and beaches and ended in-door dining. The mayor also banned large gatherings, warning residents to engage only with household family members—and to continue practicing all forms of social distancing even then.
I decided to cook a birthday dinner and invited just my immediate family to the gathering. There would be only six of us present, and my children and siblings assured me they, too, had been diligent in following guidelines. We were tired of talking to each other through video, and since Thanksgiving, Christmas and Kwanzaa gatherings were off the table. What could be the harm of enjoying each other’s company for two or three hours?
Three days later I got the answer. My son, who had traveled several hundred miles to join us, was the first to experience symptoms. “Ma, I think I got coronavirus,” Yusuf said in a call, his voice was raspy and weak. “I took the test, I hope it doesn’t come back positive, but I’ve never felt this sick in my life."
“Everybody needs to get checked. I’m the only one in my house that has it so I had to have caught it up there,” he said.
And then, one-by-one, over the course of 48 hours, each of us began experiencing symptoms too. I was the last one. It started with a bout of light-headedness, followed by extreme bouts of fatigue and a fever that produced cold chills. I braced myself.
To relatives, I embodied the image of Black motherhood—confidence, strength and courage in the face of adversity. But I was also scared out of my mind. Black folks did not fare well with this disease. According to the Illinois Department of Public Health (IDPH), 1.3 million people were infected. Of that number, 133,581 were African American and nearly 4,000 of them died. The first victim in the state, retired nurse Patricia Frieson, 61, died March 16, 2020. Her sister, Wanda Bailey, 63, died nine days later. By April, 70 percent of all COVID deaths in Chicago were African American.
On February 6, California resident Patricia Dowd, 57, became the first U.S. citizen to die of the Coronavirus.
For two and a half weeks me and “Rona,” my nickname for the pathogen, played matador and bull. If I was the bovine, then this serial killer would not win. Some days with ‘Rona were better than others—at least I could breathe, work or do chores and feel like myself for a while. But just when I thought I should have been coming out of the disease’s grip, I suddenly took a turn for the worse. The matador struck. One day I felt normal, and then the next, I could barely get out of bed.
Though my breathing remained normal, lethargy shrouded me like a blanket. I felt like I had been climbing Mount Everest barefoot and in a hailstorm. Everything hurt except my eyeballs. I’d fall so deeply asleep that I’d set alarms to jolt me awake, afraid the matador would kill me in my sleep. Unlike the hulking bull, I was fully aware of what my tiny opponent was capable of, and so I was prepared to fight—it was my life or ‘Rona’s. I tried to keep myself encouraged.
The COVID horror stories were everywhere like bad gossip and on media repeat like an earworm. Community members shared in social media their own battle tales with each offering adding to the smorgasbord of advice on how to beat it. Now that I had it, I didn’t know what to believe.
I told myself that all I needed to do was to stay nourished and hydrated. My senses of taste and smell were nowhere to be found and so I had no appetite. Still, an empty stomach didn’t stop me from throwing up.
I knew I needed to eat, so I asked a relative to bring me a few cans of soup. “I think I can keep it down. I’ll leave the door unlocked,” I promised in a short phone call. My speech was slow and my voice was raspy. It hurt to even think about forming words. “That way you don’t have to come in contact with me. Just wear your mask, put on some plastic gloves. Come inside and put the bags in the kitchen. I’ll get them after you leave.”
With some effort, I mustered enough strength to get out of bed and unlock the front door to my home.
The next thing I remember is being roused awake, hearing the wail of sirens and realizing I was in the back of the ambulance. The second thing I remember is scanning myself, thanking the Lord that I had on clean clothing, clean underwear and clean socks. Mama had always warned us about the need for such things. “You might get hit by a car,” she once mused, “and I don’t want you all embarrassing me!”
Being roused from unconsciousness is nothing like being awakened from sleep. I was disoriented, confused and trying to figure out who the three white men were who were yelling my name and hovering all around. I did my best to answer their health assessment questions.
Then I focused my eyes on the faces of the paramedics. As assuring as they looked, that didn’t stop me from trying to thrust myself upward as if I were an Alvin Ailey dancer doing a sauté’. “It’s okay ma’am,” one of the paramedics said, as he gently pushed me back down by my shoulder. “You’re going to be okay. We’re taking you to South Shore.”
The paramedics quickly explained that 911 had been called because I was found passed out. I remembered my loved one who had been en route to bring food. “You’re one lucky lady,” one of the guys said, and then began peppering me with a million questions. They had covered my nose and mouth with a mask and put a blood pressure cuff on my arm. I was grateful that I was less than five minutes away.
What happened in its wake was a three-and-a-half-month ordeal hospitalized and mandatory dialysis treatments, with little clarity on what was happening to my body other than I had just recovered from COVID-19.
SOUTH SHORE HOSPITAL
South Shore Hospital opened its doors in 1912 during the Progressive Era eight years before the community of South Shore became a settlement. That same year marked the birth of my maternal grandmother, who was born near an Arkansas cotton plantation.
Other notable births that year included those of historical figures such as civil rights icons Bayard Rustin and Dorothy Height, and filmmaker Gordon Parks. W.C. Handy recorded a hit with “Memphis Blues,” and in October of that year, former President Theodore Roosevelt was nearly killed by an assassin’s bullet, saved only because the speech he carried in his breast pocket slowed the projectile’s impact.
According to the Chicago Historical Society (CHS), the community was “a collection of settlements in southern Hyde Park Township, including the neighborhoods of Essex, Bryn Mawr, Parkside, Cheltenham Beach, and Windsor Park. The working class and upper crust community consisted of European immigrants, steel mill, and railroad workers—many of whom fled the nearby Washington Park area as Blacks and Jews moved there.
South Shore, on the other hand, was part of the city’s population explosion and expansion of its medical care ecosystems to the delight of Mayor Carter Harrison, Jr., who had just won his fifth term. “Beginning in the last decade of the nineteenth century, groups of physicians and physician-entrepreneurs established for-profit hospitals such as the Lakeside Hospital, Garfield Park Hospital, Westside Hospital, and Jefferson Park Hospital,” CHS wrote on its archival website. “Later examples of this type included North Chicago, Washington Park, Ravenswood, South Shore, Washington Boulevard, Burnside, Chicago General, John B. Murphy, and Belmont hospitals.”
In the emerging South Shore, a new medical facility was required to meet the health needs of the flux of white residents who moved to the area to escape the trickle of Black and Jewish families that moved to nearby Washington Heights/Park. This pattern of white flight, racial segregation, and economic discrimination would continue for several decades.
It would take another 56 years before Blacks and other minorities saw any relief from the federal government, the Fair Housing Act, as part of Title VIII of the Civil Rights Act of 1968. In 1974 the federal government created the Equal Credit Opportunity Act followed by the Community Reinvestment Act three years later.
Even though a few Black families migrated to what would eventually become known as the city’s “Soul Coast,” they still could not find or afford quality health care treatment and culturally competent, compassionate care other than at Provident Hospital and a few medical charities. One such charity would later be known as Cook County Hospital.
A decade prior to SSH’s launch, famed heart surgeon Dr. Daniel Hale Williams organized Provident Hospital and Training School for Nurses in 1891 in response to the lack of access for Black patients and to provide training and employment to Black physicians and nurses who were not welcomed at white-controlled hospitals.
SSH was noted as a reputable and opulent institution and maintained its status well into the 1950s as the neighborhood grew more diverse with Black families. By 1970, 69 percent of all residents were African American, and according to the U.S. Census, ten years later South Shore was 95 percent African American. The “Soul Coast,” adorned with lavish homes, lakefront ambiance and a solid middle class, had fully arrived.
Over time, the vibrant, pristine neighborhood began to look malnourished. South Shore’s commercial district along East 71st Street was downright emaciated. Racism, politics and restrictive covenants along with the loss of jobs had a helping hand in destabilizing a strong and vibrant neighborhood.
According to South Shore Works, a committee organized to advocate for community change, unemployment in the community stands at 17 percent, with at least 41.2 percent of residents reporting they are not in the workforce at all. In 2017, 20 percent of residents reported working in the healthcare industry.
More than 100 years later, the hospital sits as a shell of its grand history. According to a 2019 Community Health Needs Assessment, prepared by the Illinois Public Health Institute, the hospital’s 17-community service area includes Auburn Gresham, Avalon Park, Burnside, Calumet Heights, Chatham, East Side, Englewood, Greater Grand Crossing, Pullman, Roseland, South Chicago, South Deering, South Region, West Englewood, West Pullman and Woodlawn.
SSH employs 470 people, of which 104 are physicians, the report said. Though it is licensed for up to 170 patients, its current staffing levels allow for 135. Patients seek care at the hospital for a variety of maladies such as diabetes, HIV/AIDS services, emergency medicine, geriatric psychiatry, and detox services.
Though it continues to provide care to thousands of people annually, it’s an open secret that some residents of the neighborhood shun the place. The facility is drab, devoid of light, and looks more like a neighborhood clinic from the 1970s. Even though the hospital’s financial reports indicate it spends upwards of $1.1 million on facility improvements, it didn’t appear they had bought any paint or lightbulbs.
According to the 990 filed with the Internal Revenue Service, the non-profit paid its CEO, Timothy Caveney, an annual $240,407 in salary. Medical Director Dr. Vera Ray earned $197,319 and Nurse Manager Milicia Lukac made $188,029. Illinois luminaries such as former Cook County Board President Todd Stroger who acts as treasurer, serve unpaid on its board of directors.
When I was treated there, a few certified nursing assistants could be overheard complaining about everything from feeling overworked to not having enough staff to transport patients. At least three different nurses told me, in confidence and unprompted, to “get the hell out of here.”
South Shore’s ER department is typical of what you’d find, chaos, urgency and trauma. At one point, police and paramedics wheeled in the body of a man who had been gunned down. For roughly 40 minutes, I listened and watched as medical staff debated one another on the protocols for reporting the death to the Cook County Medical Examiner.
Their main concern was how to get the County to take custody of the body. As they debated, the family of the deceased man began banging on the locked doors leading to the ER demanding to see their loved one. While that was going on, an afflicted woman popped out of her treatment room and started stealing medical supplies that had been left unattended. She may have gotten away, except a patient in the bed next to mine alerted staff by yelling at the top of her lungs, “She’s stealing!”
At the same time, a male ER patient started his own screaming. For several minutes the man groaned, yelled, wailed and made noises that sounded like vomiting, before someone asked him to quiet down. Eventually they checked on him. By then, the staff decided to wheel the dead man into an adjacent room until the medical examiner could retrieve him.
I watched all of this unfold with mock curiosity from my bed, as I waited more than 16 hours for an in-patient room to be prepared. My blood was drawn five times. I was told I had a urinary tract infection and put on an intravenous antibiotic. However, not 30 minutes had passed when I asked a different nurse how I would have gotten that, when she replied, “Who told you that? You don’t have a UTI.”
She then took a glance at my IV and I was assured. “It’s just an antibiotic, it won’t hurt you.” I never learned whose UTI results I received, but I hoped they got the treatment they needed and are doing well today.
By the time I was admitted to the floor, I felt back to normal. I was shocked to see so many empty rooms as I was transported to the hospital’s only (alleged) COVID floor. South Shore received $6,738,712 in relief funds through the CARES Act. By comparison, St. Bernard hospital in Englewood received more than $25 million, while the University of Chicago received $159 million.
“You’re lucky you weren’t in here when COVID first hit,” a polite Asian nurse said, after taking my vitals. She told me she worked through an agency and wasn’t on staff. I’m withholding her name out of courtesy—and because she was the first person to comfort me when I cried. She actually touched my shoulder. Until then, most staff stood in the doorway to speak to me or wore something similar to hazmat suits to enter my room. “Our morgue only holds four bodies and we had people dropping dead everywhere. We had to put some in rooms. They piled up so bad.”
A different nurse, who was Black, and seemed surprised that throughout my hospitalization I didn’t require a ventilator, painkillers or oxygen shared, “You must have had a mild form of it. You need to get away from here because this ain’t it,” she said. “They don’t care about Black people here.” I thanked her for her reassuring words.
The Crusader filed a Freedom of Information Act request (FOIA) to determine how many patients died of coronavirus at South Shore. At press deadline the information had not been received.
When I asked to be released, I was told there was a “state law that required patients to have two consecutive, negative COVID results before they could be released.” I hadn’t heard that one. It was reasonable that doctors would want me infection free before releasing me to the public, but how could they keep someone hospitalized in a medical unit for that length of time during a pandemic.
As I lay in my hospital bed, feeling fully recovered, I begged nurses on my COVID floor to keep testing me. I wanted out. I felt fine, the COVID-related pneumonia had been cured, but now I had a set of red, white and blue jumper cables hanging out of my chest. I had taken three coronavirus tests, one came back negative, the other said inconclusive, and I wasn’t there to get the third result.
I was told by the hospital social worker that the only dialysis center she could find was a Fresenius clinic in the Burnham Park area. After explaining they were the “only clinic to take people with COVID,” she then hit me with an uppercut when she explained there wasn’t a seat available.
“So am I supposed to stay in the hospital until there’s one open?” I asked.
“No, I’m going to discharge you to a nursing home that can give you dialysis there,” she explained so nonchalantly as if she was just ordering a pizza. “I’m sending you to Symphony in Crestwood, IL, and then you’ll be there until a chair opens at the Fresenius.”
The last time I had been in Crestwood, it was 2007 and I was an aide to Cong. Bobby Rush (D-1st District) and we were working with residents to clean up the city’s polluted water system. The city had become a cancer cluster and then-Mayor Chester Stranczek and other trustees seemed oblivious to it.
I was mortified, no, I was horrified, no I was in a panic. A nursing home 20 miles away from my home? I’m not old enough to be in a nursing home. My family won’t be able to get to me. Who picked this place? I thought of my father and the scores of elders I met at his facility. I told her to find another option but she declined, explaining, “Here’s the problem. You have a catheter in your chest. You’ll need dialysis the rest of your life and you need treatment every other day. I can’t send you home. Symphony has an in-facility dialysis center. You’ll be fine.”
“But didn’t Symphony just get sued?” I pleaded “if I must go to a nursing home, why do I have to go all the way to Crestwood?”
As the pandemic spread, Illinois Governor J.B. Pritzker and 14 other governors took action to limit lawsuits over deaths, injuries, infection control, inadequate staffing and other COVID-related decisions at nursing home facilities. The act essentially gave senior care facilities operators a sort of “immunity.”
NURSING HOME HORROR
With no other options available to me, I turned to SSH’s medical staff and begged them to do all they could to send me home rather than a nursing home. Claiming the decision was either “above their pay grade” or “out of their hands,” I relented; and soon I was transferred via ambulance to Symphony at Crestwood.
Before leaving South Shore, I asked if a relative could bring me a cell phone, my identification, some personal care items and a change of clothing. I had been at SSH for over two weeks and other than a hospital gown, only had the clothing I was brought there in. I didn’t even have shoes. Thankfully they agreed and the family left the items with security. At least I’d be able to call family if needed.
I entered the facility during a holiday weekend. Though the place was beautifully decorated for Christmas, it smelled dank and old and full of sickness. I was put on a COVID unit and told to keep the door to my room closed at all times. I arrived in the evening and as I settled into the sweet and musky smell of death… an attendant burst into my room and asked to do a full body search.
He said it was protocol to check a patient’s body, including genitals, when they were admitted.
“No thank you,” I said to him. “I’m just here to get dialysis. I should be going home in a day or so.”
The man, though polite and professional, reiterated the policy. When I told him I was not going to permit a man to check my vaginal area, he told me he’d find a female. He abruptly left the room and returned with a CNA. I explained to her that there was nothing wrong with my body. I had no injuries, bruises, or scarring. I explained why I was transferred there. She looked embarrassed and said she had to do her job. The good news is she was smart enough to recognize the look in my eyes. Attempt it at your own risk.
On the bright side, Symphony served its residents a fabulous holiday meal—a cold, uncooked hotdog and with seven or eight tortilla chips. At least one of mine appeared previously chewed.

It didn’t take long for me to realize Symphony at Crestwood had no intention of providing me with dialysis treatment. Though the facility had a center, there was no staff around to administer treatments. There was nothing anybody could do, except sit there and wait for their patients to die. After all, most dialysis patients need treatments three or more times per week. If they weren’t able to get them, surely they’d wind up in dire straits or worse.
I was determined, that wasn’t going to happen to me. I started recording conversations and snapping photos. If anything happened, I wanted my family to have proof. For four days I sat trapped in the facility, falsely told that “tomorrow” I’d get the medical care I needed. Tomorrow never came, so I called a Lyft, went home to change clothing, and then called another rideshare driver to take me back to the hospital.
At South Shore Hospital the nurses greeted me with surprise. Well, rested and simply waiting for two consecutive negative COVID tests, I let them and anybody else who’d listen know that I had had enough with the medical games. Until you locate a treatment center, I do not intend on leaving this hospital. I wound up staying another two weeks.
My days consisted of getting blood drawn, pacing the floor, and finishing a volume on the life of Adam Clayton Powell.
By the time I finished the 476-page book, I was fed up and ready to leave. After several unsuccessful attempts to reach the social worker via hospital phone, I donned my mask and walked down the long, empty hallway to her office and signaled her from the door? [This woman was sitting there letting my calls go to voicemail, I fumed, the nerve.]
Less than 30 minutes after leaving her office where I used the Socratic method to have her walk me through her thought process, South Shore’s social worker on duty called me to say she’d actually found an open chair at a far South Side Fresenius center that could treat me.
It didn’t matter that I didn’t have COVID anymore, I still needed two consecutive negative tests in order to receive dialysis care in my city.
It didn’t take long for me to realize that her policy was created by Fresenius and had nothing to do with the CDC guidelines. I wondered why in a city as large as Chicago was there only one center that was providing blood filtering care for patients? Wouldn’t a hospital as established as South Shore have an array of options because of the pandemic?
It would take a while for me to develop a hypothesis about Fresenius’ relationship with South Shore. I was weeks away from learning that two federal whistleblower lawsuits had been filed against the corporation exposing the dark underbelly of the dialysis hustle.
Reporters Nairobi Henson and Shayla Simmons contributed to this story.