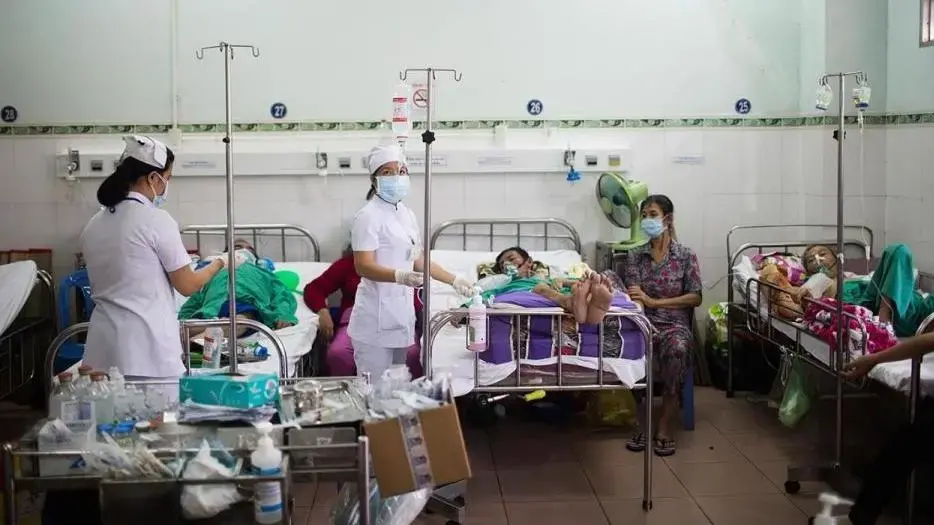
Tuberculosis is not a disease of the past. It is a disease of the poor, Pulitzer Center grantees Jens Erik Gould and David Rochkind report in a story for Slate, published on March 24, 2015, World Tuberculosis Day. Why is a disease that in one year killed as many people in Guinea, Liberia and Sierra Leone as did Ebola both under-reported and under-funded?
Jens and David's project The Price of Health: TB Budget Gaps in Vietnam explores efforts to fight TB in Vietnam mean that there's no end in sight to this infectious disease, he world's second-deadliest after HIV/AIDS. According to Rochkind and Gould, once diagnosed, Vietnamese TB patients have a 92 percent treatment success rate. But prevention, education, and detection efforts are poor. Because of this, "nearly half of TB cases go undetected," and the incidence rate remains outrageously high: 147 people per 100,000 inhabitants.
Currently, Vietnam has less than 30 percent of the funding needed to fight TB. Creating an effective triage process could make the existing funding stretch further. Additionally, rural patients often suffer in silence since they cannot afford to travel to clinics in larger cities. A faster and cheaper diagnostic test would mean that local healthcare workers could identify which patients don't need treatment without subjecting them to unaffordable or unattainable testing.
Targeting treatment to patients who really need it not only helps in the short-term, but also in the long-term, by decelerating the rate at which drug-resistant strains of TB develop.
As Pulitzer Center grantee Meera Senthilingam reports, South Africa is currently one of only two countries worldwide with rising infection rates of tuberculosis. Lack of access to healthcare has led to the evolution of "extensively drug-resistant tuberculosis (XDR-TB), a form of the airborne disease that is resistant to the four main groups of drugs used to treat it."
80 percent of the drug-resistant strains are due to airborne transmittance between people, according to Senthilingam, . This means that a large proportion of the TB outbreak could be reduced simply by developing more effective on-the-ground detection methods. For those who are unable to receive treatment, their home becomes a makeshift hospital ward—with the perfect conditions to incubate and transmit the infection.
The reality of this inaccessibility of treatment to poor and developing communities propagates the association of tuberculosis and poverty. And this stigma can be just as deadly as drug-resistant TB.
In Moldova, it is estimated that one out of every ten patients defaults on their treatment plan due to lack of education, fear, misinformation and shame associated with tuberculosis. An earlier project by David Rochkind, Moldova: Fighting a Deadly Disease, looks at the country as a case study, using it to predict the devastating effects of ineffective efforts to cope with the TB crisis. As reported by Rochkind, "the country's Ministry of Health estimates that the number of people dying from TB has quadrupled since 1994."
New testing methods for TB are still in development, but one thing is for sure: quicker and more cost-efficient detection will help to target the problem at its source—poor and developing communities with limited access to medical care.

Tuberculosis is the leading cause of death in South Africa. Drug resistance is now so strong that...









