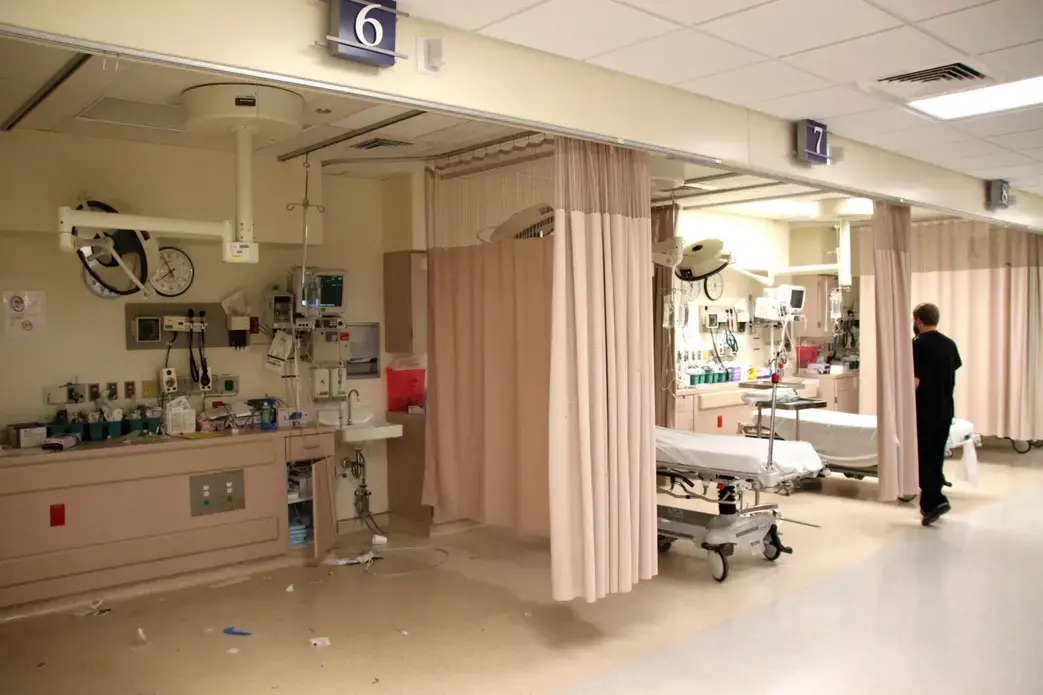
It's early when the call comes in, not even 2 p.m.: Man with multiple gun shot wounds arriving shortly. Not your average time for a shooting in the streets of Chicago. But working in one the busiest trauma units in the country you don't count on "usually" and "in general." You are prepared. And the staff of John H. Stroger, Jr. Cook County Hospital is just that. Within minutes the heart of the trauma unit moves from the center of the floor to one of the two available shock rooms.
Surgeons and nurses prepare calmly and efficiently, putting on extra scrubs, getting equipment and medicine ready. The paramedics already started CPR to try to restart the patient's heart. When they arrive, a physician takes over, and nine people get to work. Try everything. Push adrenaline in an attempt to force the heart to beat again. This time they don't succeed. A surgeon calls the time of death at 2:17 p.m. A single sneaker lies lost on the floor next to empty foil packages and bloody bandages. The patient had at least 11 gun shot wounds.
Nothing exceptional for the team around Dr. Kimberly Joseph, who has been an attendant at the trauma unit since 1993. Stab and gun shot wounds account for 30 percent of the patients at the public hospital. Last year 5,700 patients were treated in the 14 available beds here at the trauma unit. For the six full-time attending surgeons, the two burn surgeons, the multiple residents and nurses, the cause of the injury is secondary. "We look at how the patients are doing and not how they were injured," says Dr. Joseph.
An observation area as well as an intensive care unit are part of Stroger's trauma unit. The flow of patients is steady. Three more gun shot wounds and a patient with third degree burns in critical condition are among the cases that come in on a day that is considered slow by those who've seen all beds in the unit being occupied.
Tyrone says he has been shot several times. He is 22 years old; the wounds at his left elbow are constantly bleeding. "Have you been shot before?" "No." "Have you been drinking?" "No." "Do you smoke?" "Only weed, no tobacco." Standard question for the physicians but they can never be sure if the given answers are true. "Sometimes people forget that they have been shot before," says Dr. Liz Gwinn, a five-year resident at Stroger.
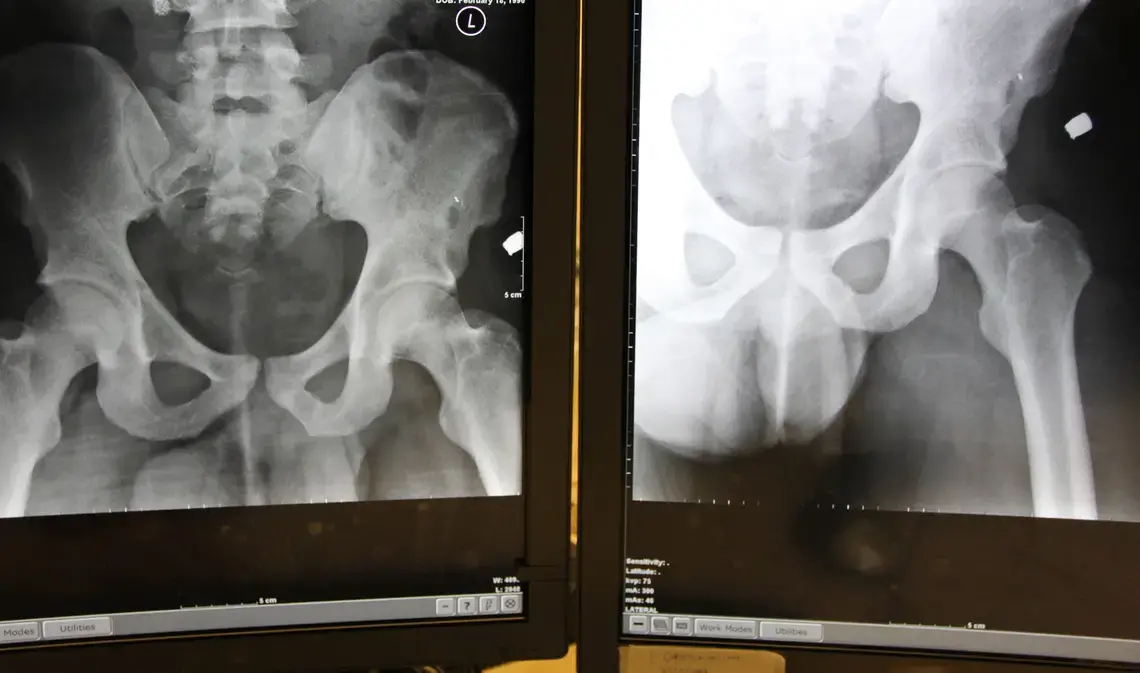
For Tyrone though, it's a first. The doctors find three wounds in his arm. Not a good number. Two would be better. Or four. Bullets have an entry and an exit wound, an even number. An uneven number means that the trauma team has not found every wound, yet. Or that one bullet is still inside Tyrone. The arm needs to be moved––Tyrone asks for more pain medicine. And for his grandmother. But the examinations come first. An X-ray shows that fragments of a bullet are sticking in his elbow close to the bones. Tyrone needs to have surgery. But he has to wait until the next day––his condition is not critical; at night the operating rooms are reserved for those patients whose lives are in danger.
After the police have gone, and the medical staff has fixed Tyrone's arm for the night, he finally sees his grandmother and sister. "I don't know who shot me," he says. He claims it must have been a mistake. It always seems to be a mistake. "I just want to leave this violence behind," says Tyrone. But after the surgeons fix his arm he will return home, back to the crime scene.
Fixing a patient in the trauma unit should normally be the start of the recovery process, but those suffering from gun shot wounds are from the poorest neighborhoods of Chicago. They often are under-insured or not insured at all. Their troubles are just beginning.
"Your idea of life changes if you are threatened at home," says Dr. Charla Waxman, who is an instructor for Mental Health First Aid, a program that teaches social workers, teachers and others to help children who have developed a mental health problem––a problem that is underrated when it comes to the trauma of gun violence. "There is still a stigma connected to mental illness in this country," says Dr. Waxman.
Working at a trauma unit can be a frustrating job--emotionally hard, although all surgeons agree on one thing: Leave the job behind as soon as you leave the hospital. A rule Dr. Frederic Starr normally follows. But the married father of two kids also admits: "It can be emotionally hard especially if it's kids because they are really innocent." Starr has been working at the trauma unit for ten years and says he loves the job as every patient is different and nothing ever is the same. "I have seen miracles happen," Starr says. On this Saturday night so far no miracles are needed.
A 23-year old who is hospitalized shortly after 9.30 p.m. is in stable condition. But once again the numbers don't add up. The team finds five wounds in the left upper leg close to the hip. An uneven number. The search begins. And a bullet can travel far. The first X-ray shows the whole bullet sticking close to the patient's hip deep underneath the skin. "We won't remove it because we could cause more damage to get it. We would have to make a large incision," says Dr. Gwinn, who is on call again this night. The 31-year old will be a trauma fellow starting in July. She changed her goal of becoming a pediatrician after she first stood in an OR and saw how trauma surgeons can fix things. In Chicago, where 43 people were killed in January alone, that means a lot of fixing. "It is actually ridiculous how many gun shot wounds we are seeing here," says Gwinn. "But we all love to do this work."
And they treat every patient the same, no matter what. The 23-year old with the gunshot wound wears an electronic ankle bracelet on the same leg that has been shot. He was just released on parole. Later, the police will say that the patient was shot while sitting on his porch and that he supposedly knew the perpetrators. The surgeons and nurses are not aware of any of this while caring for the patient. "I treat every patient the same and sometimes I don't want to know and sometimes it is better not to know what happened," says Dr. Starr.
On this Saturday night everybody gets lucky. No more patients with gun shot wounds are admitted. A quiet night for the city. But just spending a couple of hours observing the work of the surgeons and nurses you see just how much trauma a bullet causes.
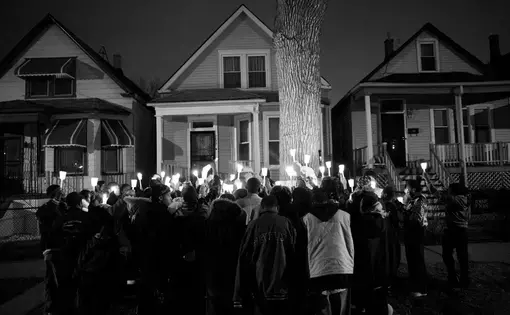
Education Resource
Rieke Havertz on Chicago's Gun Violence, from a German Perspective
Rieke Havertz is an editor and writer for the German newspaper Taz, Die Tageszeitung. With a degree...