
It’s thought that Covid-19 originated in animals before jumping to humans. Now experts are warning that the chances are the next pandemic will, too.
Seventy-five percent of the newly emerging diseases currently affecting people originate in animals, according to Predict, a US government-funded collaboration by infectious disease experts across the globe. Already, Predict scientists have identified 1,200 new zoonotic, or animal-borne, diseases. But scientists estimate there are some 700,000 more zoonotic diseases we don’t even know about yet.
One animal that is capturing scientists’ fascination – and fear – is the camel.
Across northeast Africa, Asia and the Middle East, humans raise these long-necked, hump-backed mammals by the millions. Entire societies rely on camels for milk and meat, weddings and wealth.
Their owners often describe them as gentle creatures. But try approaching one with a needle to take blood samples or with Q-tips to take nasal and rectal swabs, and you’ll quickly discover their wrath.

“It could kick you. It could spit on you. It could urinate on you,” says Millicent Minayo, a surveillance officer with Washington State University who for two years has been spending her days taking samples from camels and herders in Marsabit, Kenya. “And anyone who is in contact with them could get that infection.”
“That infection” is Middle East respiratory syndrome (Mers), a novel coronavirus that so far has proven to be at least 10 times more deadly than Covid-19. It was discovered in Saudi Arabia in 2012. By 2016, the World Health Organization (WHO) had identified “1,761 laboratory-confirmed cases of infection with Mers-CoV, including at least 629 related deaths.”
Later that year, an outbreak at a hospital raised the alarm that it’s not just camel herders who are susceptible to the disease, but anyone at all.
But while camels can be carriers, the Mers threat to humans is mostly man-made. As human-induced climate change makes droughts more frequent, prolonged, and severe, herders have had to abandon cows and other livestock for camels because only they can survive weeks without water. The result is a growing number of camels in close contact with humans – the perfect conditions for the spread of a deadly disease.
“We brought this study to Kenya because we have a huge number of camels. And especially in Marsabit,” says Minayo. Already, she and her colleagues have encountered the virus in camels – about 14 in 2019 alone, she says.
Now they’re racing to test for the virus among humans in the hopes of stopping its spread before it can escalate into a pandemic like Covid-19 – one that could threaten not just herders in Kenya, but people around the world.
“You don't know how this disease, if it gets to the humans, how it will go,” says Minayo. “Nobody knew that this Covid-19 would create a global pandemic which has claimed lives of so many millions of people. So, it would be a good thing if we could prevent rather than treat.
“Prevention is better than cure.”
Camel country
Kenya is home to 3 million camels – nearly 10% of all the camels in the world, and more than any other country but Sudan and Somalia. According to the Kenyan government, Marsabit is home to at least 224,000 of them. That’s nearly as many camels as people. Marsabit is Kenya’s largest county by land, but one of its smallest by population, with a mere 1% of Kenyans calling it home.
Eighty percent of them live in poverty. Marsabit’s economy doesn’t benefit from many of the industries that keep other parts of Kenya afloat, such as tourism – of the 2 million tourists who visit Kenya each year, only a few thousand make the journey to Marsabit.
On the outskirts of town, dozens of women in brightly-coloured clothes wait outside a gate to the National Cereals and Produce Board. Since Covid-19 forced Kenya’s economy into a partial lockdown, each morning the women line up in the hopes of being hired for a few hours’ work packaging food – maize, sugar, rice, cooking oil – to distribute to hungry families who lost their income due to the pandemic.

Livestock accounts for 85% of Marsabit’s economy. As well as providing an economic livelihood, camels and cows can be family assets, used for expenses like dowries or school fees. Both animals are often seen as more secure investments than sheep, goats, or other livestock, which live for fewer years. Camels, in particular, are becoming more common as herders turn to a sturdy animal that can survive increasingly frequent droughts.
But the more camels there are, the higher the risk of zoonotic disease. “Moving growing numbers of livestock across the landscape increases interaction with wildlife. Diseases can jump from wildlife to your livestock, and from there to humans,” says Dawn Zimmerman, a wildlife veterinarian with the Smithsonian Conservation Biology Institute’s Global Health Program who leads Predict projects in Kenya.
“The diseases are out there. Given the opportunity, they could jump.”
Mers already has. One recent study found that camel handlers are particularly vulnerable to Mers – and that some even tested positive for antibodies, meaning they’d already been exposed to the virus.
To trick a camel, it’s all in the tail
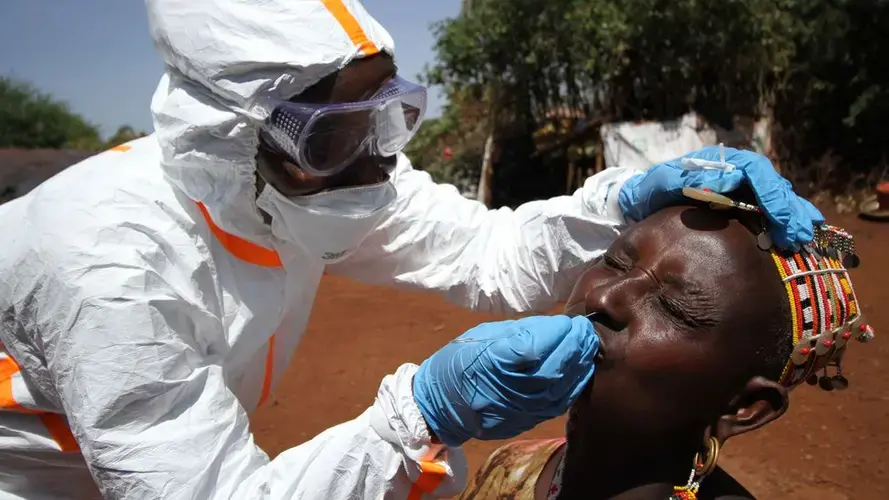
Each morning when Minayo and her colleague Boru Dub Wato set out to test camels for Mers, they take precautions that the herders themselves cannot. Goggles. Facemasks. Full-body dust coat. Face shield. Gum boots. Gloves. By the time they’re all suited up, they look comically out of place – like a pair of Ghostbusters about to de-ghoul a rural African village.
They call upon herders to round up six unlucky camels for testing. The camels are calves, each less than two years old, but they tower over their owners as they begin the thorny process of holding the animals down.
“They are huge animals,” says Dub Wato, who grew up around camels as a Marsabit native of the Gabra tribe. “You need power” to restrain them, he says. Even so, you’ll never succeed “unless you use a lot of tricks.”
The first trick is to start with its tail – once you grab hold of it, the camel can’t run away. “The other person can go for its ear. Then, you hold it by its lips,” Dub Wato says. The camel makes loud, hee-hawing groans like a donkey while it tries to kick or to knee its captors. Dub Wato swabs the camel’s nose, then its anus. Then he uses a needle to take blood from just behind the camel’s jawbone.
After all the camels are sampled, it’s the people’s turn. One by one, children sit on a chair making faces of disgust while Minayo swabs their noses and throats. When an elderly woman with a smile takes the hot seat, Minayo asks her age. A friendly debate ensues. The woman’s birth year was never recorded. One relative says she’s 90, another argues she’s more like 110. The children laugh. “Just write down 100,” says another. Minayo obliges.
Their field work finished, Minayo and Dub Wato take off their personal protective equipment and ferry the samples by motorcycle to a lab in town. There they place the blood in a centrifuge, then package it along with the swabs into a bin filled with liquid nitrogen to cool the samples to -80C for the long ride to Nairobi, where the swabs will be tested for Mers.
Medical crisis in the making
Even before Covid-19 arrived, 13 different zoonotic diseases, including tuberculosis, hepatitis E and avian flu, were causing 2.4 billion cases of human illness and 2.2 million deaths each year. Many of these diseases are transmitted by livestock. In poor countries, 27% of livestock show signs of past infection by zoonotic disease, and one in eight animals becomes infected each year.

In Kenya, reminders of the risk are ever-present. In 2017, a mobile-phone data collection system successfully alerted health officials to an anthrax outbreak among buffalo, allowing the country’s government to stop it before it could endanger humans. It’s part of a national programme being developed to stop the spread of zoonotic disease.
Meanwhile, in Mandera county in May 2020, at least 70 camels died from an unknown ailment. And in 2019, there was an outbreak of Rift Valley fever, a deadly disease that spreads when humans come into contact with the blood or organs of infected cows. Fortunately, no one died.
But luck is not everlasting. In June 2020 in Meru county, near Marsabit, at least two people died and nine were sickened by what doctors suspect may have been another, animal-induced outbreak of anthrax.
And in 2014 in Marsabit, 139 people died from Brucellosis — a highly contagious bacterial infection that is easily transmitted through unprocessed milk or undercooked meat. Already, brucellosis infects one out of every eight cows in the world. But fewer than 30% of herders and farmers know how brucellosis gets passed from livestock to humans, according to a recent study led by Kariuki Njenga, who is also the lead scientist on the Marsabit Mers field study on behalf of Washington State University. Herders, in particular, were likely to engage in high-risk practices like drinking raw milk or handling raw hides.
So far, Mers has not jumped to humans in Marsabit. All of the swabs from people that Minayo’s teams have tested in the last two years have been negative. But if – or when – it does, it could be devastating.
“Among humans, it is a very deadly virus,” says Minayo. “When there is human to human transmission, you don't know who will get it. It could land on those who are immunocompromised. It could land on the children whose immune systems are still growing.”
Mers causes the same sorts of respiratory system complications as Covid-19, including pneumonia. Symptoms often start with nasal congestion, a cough, chest pains, or difficulty breathing. In the worst cases, it may cause fibrosis — irreversible scarring — in the lungs. This can be deadly. More than one-third of all humans known to have contracted Mers have died from it, according to the WHO.
While we’ve seen from Covid-19 how an outbreak can catch health systems around the world unprepared, Marsabit risks being particularly overwhelmed. As of 2014, there were just five doctors in all of Marsabit county — one doctor for every 64,000 people. That’s 64 times the WHO recommended ratio of one per thousand.
But the threat goes far beyond Marsabit.

Some scientists say Mers could pose a risk to humans all over the world – starting with wherever camels are found. Far from Kenya in the Gobi Desert of China and Mongolia, wild camels are coming into increased contact with humans and livestock, making them more vulnerable to Mers. In Morocco, meanwhile, a 2019 study discovered Mers antibodies among camel herders and slaughterhouse workers, suggesting that the disease is “high-risk” for jumping to humans there as well.
Once it jumps from animals to humans, a Mers outbreak could grow rapidly. Saudi Arabia alone saw 15 people infected in December 2019 and January 2020 — three of whom were hospital workers infected by their patients. “The fact that RNA viruses such as coronaviruses mutate means you never know what could happen with that particular virus,” says Zimmerman.
That’s why it’s so crucial to fund research to identify the animals and diseases that could cause the next regional or global epidemic now, says Zimmerman. “It’s important to know what’s out there,” Zimmerman says.
If, or when, Mers jumps from camels to humans in Kenya, “there is no contingency plan in print,” says Njenga.

Rather, health workers in the Marsabit region have been trained to “pretty much use the Covid-19 playbook: Isolate the person (and) wear PPE,” or personal protective equipment, to keep themselves from becoming infected, says Njenga. Health workers also will have to conduct contract tracing as quickly as possible — just like much of the world is doing now with Covid-19.
Herders are likely to be the first victims, says Minayo. “Camels too sneeze and cough. When it spits on you, when it sneezes … anyone who is in contact with camels could get that infection from the droplets,” she says.
And unlike humans, she says, “camels don’t wear masks.”
A lifestyle of risk
One sunny morning at her homestead in Marsabit’s Karare district, Ng’iro Neepe milks each of her family’s female camels, called dames, by hand. When I ask Dub Wato to translate my question to Neepe about what she would do if disease killed her camels, she smiles, amused.
“Tell this mzungu that we are Samburu,” she says — one of Kenya’s 42 tribes, known for their pastoralism. “Milk is everything,” says Neepe, "mzungu" being the Swahili word for “foreigner.” “Without it we have nothing. We rely on it to get money to buy things. I drink it, I cook chai, and I sell it.”

Each night that herders spend away from their homesteads, seeking grass for grazing, is a night they sleep with their camels for warmth. By day they drink camel milk raw — sometimes their only source of sustenance for days or weeks at a time. When a camel dies in the desert, herders sometimes eat the meat without cooking it, for lack of firewood.
All of these actions risk spreading the virus.
“We tell them how they can safeguard themselves,” says Dub Wato. “Avoid close contact, and when contact is necessary, you can have a mask on. Once you’ve had close contact, clean your hands or sanitise — just the same way we are doing it for Covid-19.”
In Kenya, most camel milk is consumed raw, which can spread disease. Dub Wato’s team urge herders to boil their milk before drinking it. Some herders have taken heed. “Before you guys came to tell us, we didn’t know that there were diseases from milk,” Neepe’s brother, a herder named Lemilayon Lekonkoi, tells Dub Wato. “We just drank milk raw. But since we were told, now we boil it.”
In order for me to taste it for myself, she carries a fresh container into her short, thatched roof hut, lights a small fire, and begins boiling camel milk chai. The milk is fatty, with a sweeter taste than cow’s milk. Most Kenyans enjoy their daily chai with a heap of sugar. But here, many drink camel milk neat, with a frothy top layer.
Marsabit’s camel herders may soon enjoy hot chai less regularly. “Drought frequencies have increased to every one to three years, during which pastoralists can lose up to 50% of their herds,” found a report by the Kenyan government. “In many areas, extreme events and variability of weather are now the norm.” But climate scientists say the worst is yet to come: The UN predicts that temperatures in Kenya’s will rise by 2C by 2050, and by 2100, some parts of East Africa may see a more than 50% increase in land affected by drought.
Already, those increased droughts have forced herders to wander further into the desert in search of grass for their livestock to graze — and so they spend more and more of their time away from their homes, without fire, says Njenga.

Still, the scientists in Marsabit say behaviour change alone cannot solve everything. Many herders have no choice but to live in close contact with their camels. And some still drink camel milk raw when they’re out in the bush.
A camel’s climate
Like cows in America, pigs in Europe, and the other animals we eat around the world, camels are curated for human consumption — bred, raised and grazed for milk and meat. “These animals that we keep, we are not keeping them as pets,” says Minayo. “They are our means of livelihood.”
Many experts believe that the risk of zoonotic disease is likely to rise as more animals are raised to feed more people and as climate change forces them onto new frontiers. Climate change brings another consequence, too: as droughts become more frequent, more herders are turning from other livestock to rear hardier camels instead. Of 400 families of the Borana tribe surveyed in one 2014 study, 41% said they had stopped rearing certain livestock due to climate change, while 71% said camels were their animal of choice due to how long they can go without water.
“I have started keeping camels only recently,” says Lekonkoi. He switched from cows on account of camels’ ability to withstand the more and more frequent droughts. He has no regrets. “Everyone now sees the importance of the camel,” he says.
But camels may pose a greater risk to humans than other livestock, largely due to their lifespans. Dairy cows tend to be slaughtered after about six years, meaning a cow infected with Brucellosis, for example, has a limited time to transmit the bacteria to humans. Goats and sheep live as little as two years. But a camel infected by Mers or other diseases can remain a risk throughout the animal’s 15- to 20-year lifespan.
Lekonkoi knows Mers by its colloquial name — Homa ya Ngamia (camel flu) — only because Minayo and Dub Wato have warned him of it. He believes he’s seen the disease affect camels nearby. “We see them coughing — just like human beings. But we just live with them, with their coughing,” he says. “We can’t run away from them.”
This is the tension at the heart of the battle to prevent Mers’s spread. Marsabit’s herders depend on their camels to survive. But scientists believe that as the herders face increased droughts and harsher climates, their risk of being infected with a dangerous virus will grow.
Scientists are working hard to stop the next pandemic, testing camels and people alike. But in a changing world that makes it ever easier for diseases to jump from animals to humans, the question remains of whether testing and prevention will be enough.







