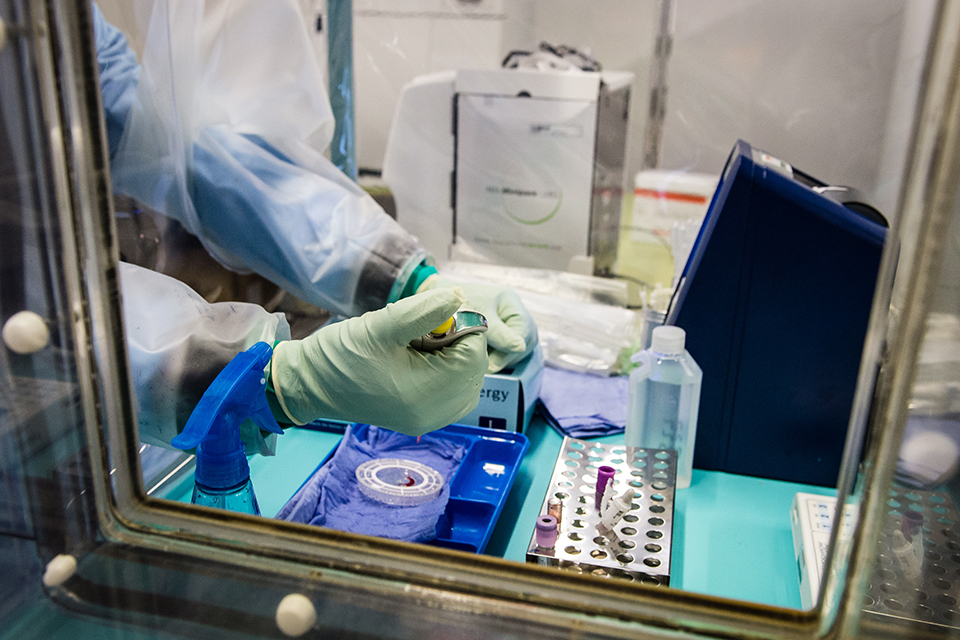
At the World Health Assembly in Geneva last week, I spoke with Jim Campbell, executive director of the Global Health Workforce Alliance, a group that works on solutions for the chronic shortage of paid, supported health workers. The group, hosted by the World Health Organization, estimates a global shortage of 7.2 million health workers.
Further, the group reports that the number of nurses and midwives decreased in 35 percent of countries already identified as having an insufficient ratio of health workers to support the population. In the US, the ratio is 118 nurses per 10,000 people. In Cuba, it's 159. In Sierra Leone, it's 5.
After more than a decade of aid to improve the health of people in many countries, why do so many of these countries still have an anemic health work force?
You need to look at the terms and conditions of health worker employment, including payment, support and supervision. If you don't treat people with appropriate respect, and pay them a living wage, you're going to have unmotivated, poor-performing staff—in any industry, let alone the health industry. These are, after all, human beings and they display human behavior.
Why has aid not gone into ensuring that national health workers get what they need for the job?
If you look at the Millennium Development Goals (MDGs), you'll see there is a preference by the international community for clear targets, such as reducing the number of deaths of children under age five. To reach this and other MDG targets, aid groups often take a project-based approach.
Take the example of the U.S., one of the largest contributors to international development: Their points of focus are around the MDGs, like HIV and maternal mortality, and congressional funds are earmarked accordingly. They measure results based on the number of persons receiving treatment, drugs delivered, and the number of health workers trained. There is no focused measurement on the capacity of the health system as a result of these interventions. For instance, are the trained health workers still working in the public sector after one year, two years, three years? We don't run our own healthcare systems in this way; we wouldn't dare it.
By not building local capacity, it's like we're trying to improve health by running the latest version of Windows on an operating system from the 1980s. It's not like we haven't thought about this before. If you look at the WHO report on Global Health Security from 2007, there was a clear warning that we need human resources and infrastructure. But the world decided it was not a priority.
Why isn't it a priority? It certainly wasn't during the Ebola outbreak. As I recently reported in Newsweek, less than 2 percent of $3.3 billion in donations to respond to Ebola in West Africa was earmarked to staff in Sierra Leone's health system.
We've created a global mentality that our investment is about saving lives, saving lives, saving lives. In some countries, nurses and other professionals who graduate with advanced degrees will work without adequate pay in a facility where there is not running water and electricity 24 hours a day, and not nearly enough medicines, supplies, and equipment.
Health workers need an enabling environment. But how do you sell this to your taxpaying population? How do you say your taxpayer money is fixing the plumbing, fixing infrastructure?
Some people in the aid community argue that target-based initiatives, such as the President's Emergency Plan for AIDS Relief (PEPFAR) did end up strengthening health systems in the 43 countries they operated in over the past decade. Through PEPFAR, the US has donated 46.5 billion in bilateral funding for HIV between 2004 to 2014.
To me, that proves that the health workers in these countries are more than capable of getting results, but the question is what is the real cost of what you are achieving? What would have happened if instead, that money went through the public sector ten years ago? Would we have even stronger health systems? We don't know because we've invested hundreds of millions into parallel systems. We've never really tried to build resilient health systems, with motivated health workers who can provide quality care. We've never said let's be revolutionary, and revolutionary is what the 21st century aid response needs to be.