KONO DISTRICT, Sierra Leone — Although one of this country's poorest districts has been Ebola-free for six weeks, the deadly virus continues to mask or hamper other health issues for pregnant women and newborns here.
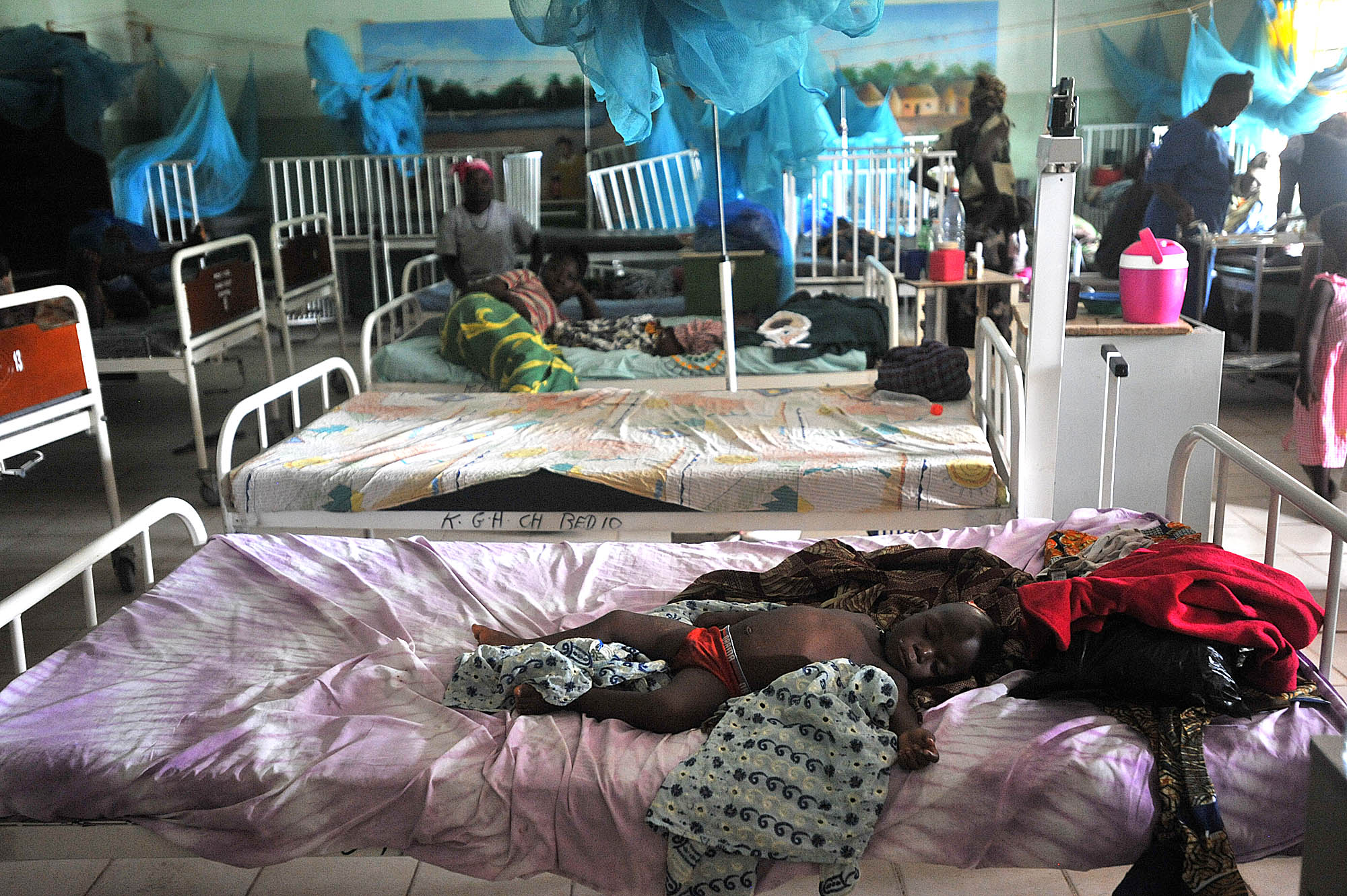
Home births without trained medical staff contribute to one of the world's worst infant mortality rates. Ebola's death toll in Sierra Leone, about 3,800, is dwarfed by the 39,000 children under age 5 who die each year, often of preventable causes like pneumonia, diarrhea and malaria, according to the World Health Organization.
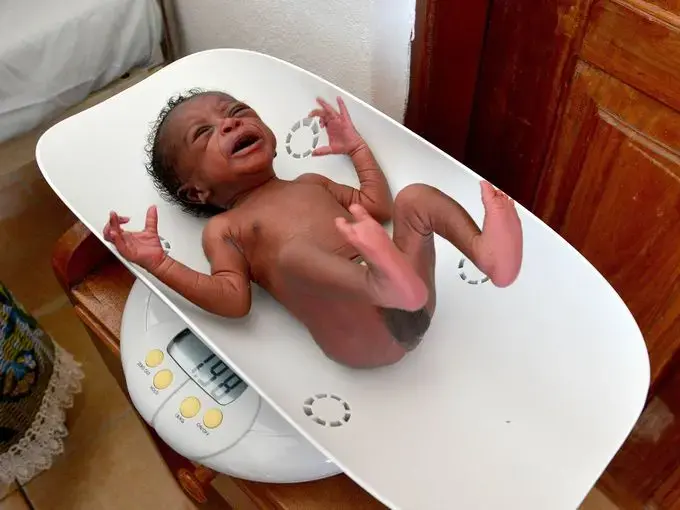
One in 20 newborns in Sierra Leone die within the first month.
Only 45% of women here use skilled birth attendants. Many women are reluctant give up ideas they associate with a child's spiritual health. For example, professional midwife Boyama Kacingor, of Kono, said some traditional healers tell pregnant women that eating eggs, a source of protein, will cause their children to become thieves.
Despite a national law that guarantees free health care to pregnant women, children and nursing mothers, nearly half of Sierra Leoneans told a survey by Transparency International they had recently paid a bribe for health services — a practice that prices some poor women out of the delivery room.
Sallie Cunceh, a driver from the city of Makeni, said he paid about $35 when his son was born at a hospital in Freetown, the capital of Sierra Leone. "If you don't give it, they will leave your wife suffering," he said. "Give them whatever they request."
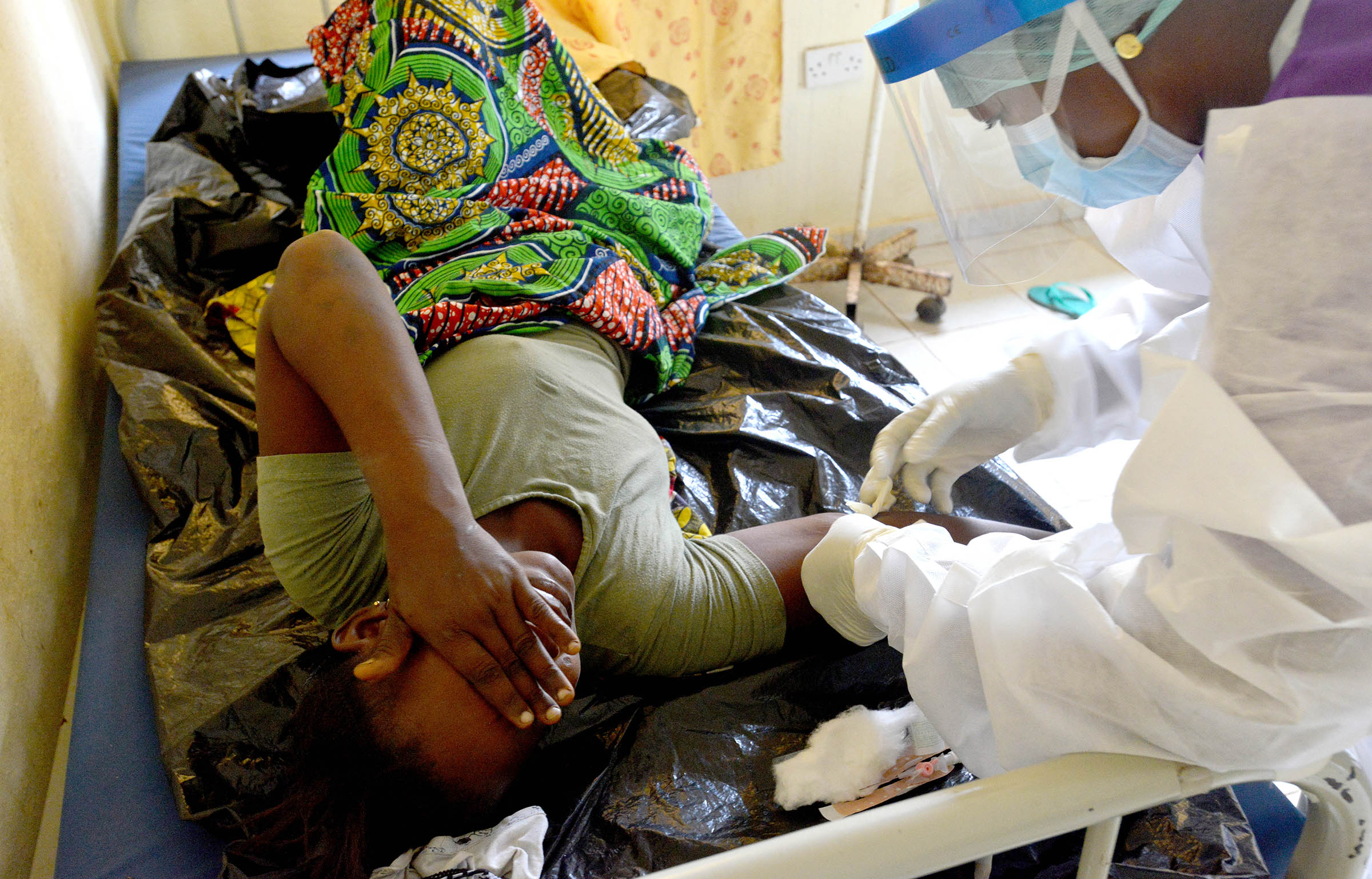
Problems of corruption, access and mistrust — all mostly rooted in poverty — limit the options for women like Salome Kamara, 27, who last week went into labor with twins. Her home has no electricity or running water, a tin roof, a dusty dirt floor and walls of mud.
With help from a traditional healer who lives nearby, she gave birth to a boy, named Lansana, on the bags of grass she and her husband use as a mattress. The newborn's cries sounded healthy in the early dawn, but the second child was breech.
The sudden complication prompted the traditional healer to ask for help from a new delivery center in Kono that had just opened. Wellbody Alliance, which has operated a health clinic for nine years, has been building trust in the community, partly by staffing the center with traditional healers from surrounding villages.
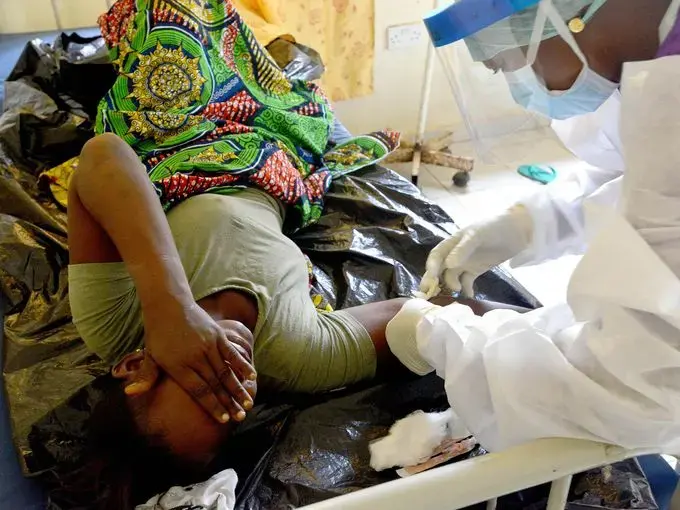
That call about Kamara triggered the deployment of a medical team that included Finda Samuel, who has delivered babies in Kono for 15 years, but is now trained as a traditional birth attendant for Wellbody.
Samuel helped deliver Lansana's brother, Alusine, who became Wellbody's first birth.
Kamara's experience serves as an example for women moving from delivering babies at home to clinical births, said Storm Portner, the clinic's co-manager of community programs.
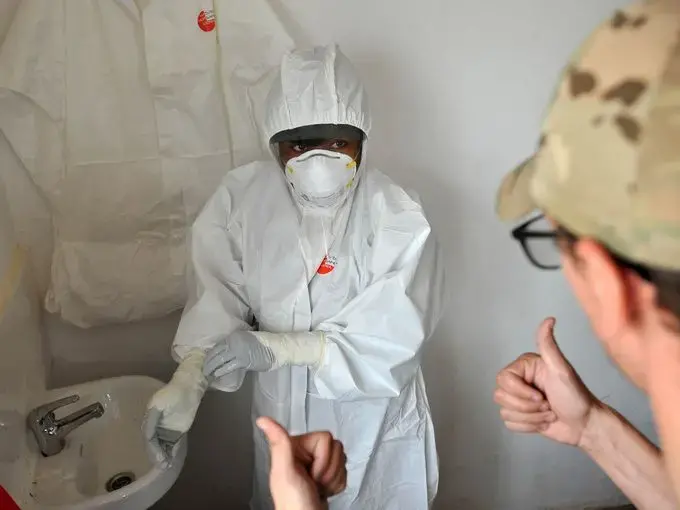
Ebola has also had an indirect effect on the clinic. The delivery center was scheduled to open last September, but delays because of the Ebola outbreak caused an estimated 600 pregnant women to be sent elsewhere, Portner said.
The main clinic has also seen its patient counts plummet because of the panic over the virus — from 20,000 in 2013 to just 11,400 last year.
A 2014 report for Kono Government Hospital, which became stigmatized after a stint as a temporary Ebola treatment center, showed the Ebola virus killed 18 children under age 5. But indirect effects prevented an estimated 3,300 newborns from being registered, a first step in getting free health care in the country.
Ronald Marsh, the hospital's medical director, said it's difficult to know how many deaths could be indirectly attributed to Ebola, but "of course, it's way more" than the 226 Ebola deaths in the district.
Meanwhile, hours after the birth of her twins, Kamara nursed Lansana on a clean bed in the delivery center. Samuel and other health workers brought her food and helped make her comfortable. And the staff gave her a lapaa as a gift — a brightly colored cloth wound around the waist like a skirt.
For future births, Kamara said, "I will choose the clinic."
Education Resource
Meet the Journalists: Matt Hongoltz-Hetling and Michael Seamans
Matt Hongoltz-Hetling and Michael Seamans traveled to Sierra Leone to document an ongoing healthcare...