Even 3 decades later, Seyed Naser Emadi's first encounter with nerve agents haunts him. In 1987, as a soldier fighting for Iran in its war with Iraq, he came across a hillside strewn with comrades killed by an Iraqi nerve agent, perhaps tabun or sarin. Unable to breathe, the victims had clawed at their necks to try to open a hole in their throats, recalls Emadi, now a dermatologist in Tehran. In fact, their windpipes were clear; the nerve agent had shut down control of breathing in the central nervous system. They "had no choice except death," he says.
The long-term effects of nerve agents remain uncertain, but with the right antidotes, these poisons need not be an immediate death sentence. A few years after Emadi's experience, U.S. soldiers in 1991's Gulf War carried autoinjectors filled with drugs that—in principle—would keep them breathing and protect them from seizures if Iraqi forces again unleashed nerve agents. They never did, most historians agree, but the threat remains real today, as chemical attacks in Syria's ongoing civil war make clear. It is spurring urgent efforts to find better countermeasures, with several promising compounds in the pipeline.
First synthesized by German chemists on the eve of World War II, nerve agents kill by binding to acetylcholinesterase (AChE), an enzyme that dismantles the neurotransmitter acetylcholine when it is released into synapses. One of the most efficient enzymes known, a single AChE molecule can hydrolyze 600,000 acetylcholine molecules per minute, says Palmer Taylor, a pharmacologist at the University of California, San Diego.
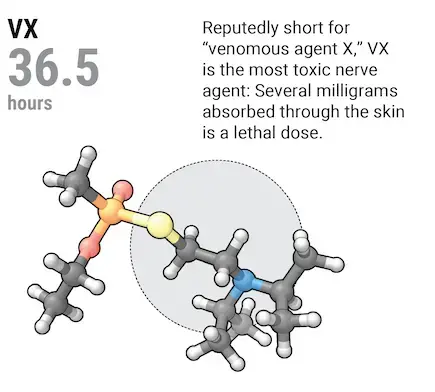
Nerve agents slot right into AChE's active center, a narrow gorge. Once one nestles there and forms a covalent bond with a serine group, AChE "can't spit it out," says James Madsen of the U.S. Army Medical Research Institute of Chemical Defense (USAMRICD) in Edgewood, Maryland. As acetylcholine builds up in the synapses, victims may develop chorea and dance ghoulishly before collapsing and writhing in seizures. Without medical intervention, the brain stops sending signals to the muscles that control respiration and maintain blood pressure: Victims drift into a coma and will probably stop breathing. Milligram amounts of nerve agents are enough to kill.
For defense against seizures, U.S. soldiers carry an anticonvulsant. Diazepam has been the treatment of choice, but the U.S. National Institutes of Health (NIH) in Bethesda, Maryland, and the U.S. Department of Defense have thrown their weight behind a faster-acting compound, midazolam. "We think it's going to be a much better drug in mass casualty situations," NIH neuroscientist David Jett says.
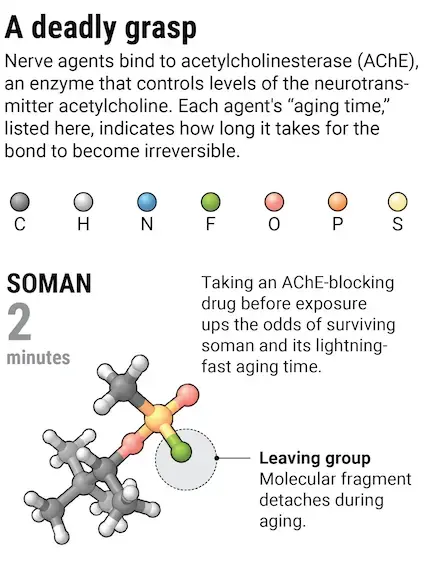
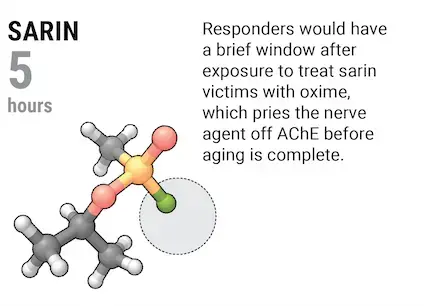
Other remedies take aim at the cause of the symptoms: excess acetylcholine. Atropine, a compound derived from the belladonna plant, blocks acetylcholine receptors and was used to treat nerve agent victims in the Iran-Iraq War. But it can't prevent nerve agent molecules that do latch onto AChE from forming an irreversible bond with the enzyme, a process measured by the nerve agent's "aging" time. Sarin's aging time is about 5 hours. Soman, a less known but much-feared nerve agent, ages AChE in just 2 minutes.
Given only atropine, nerve agent survivors need weeks for their bodies to regenerate AChE. That's why victims are also given—as soon as possible after exposure—what Madsen calls the "true antidote" for nerve agent poisoning: oximes. Like a molecular crowbar, these chemicals jimmy the nerve agent off AChE before the complex ages.
In the United States, the only oxime approved for use against nerve agents is 2-pralidoxime chloride, or 2-PAM. But because 2-PAM is positively charged, little if any crosses the blood-brain barrier, Taylor says. That's a serious drawback, because nerve agents exert their most destructive effects in the brain.
In 2001, Taylor teamed up with K. Barry Sharpless, a chemist at the Scripps Research Institute in San Diego, to create oximes that lose protons to become a neutral species; the compounds were screened for those that, once inside the brain, can regain a positive charge, which is crucial for the molecular jimmying to work. Taylor's team has tested its front-runner in mice and in macaques exposed to sarin, and in August 2017 reported that it rapidly reversed symptoms.
A group led by Carlos Valdez, a chemist at the Lawrence Livermore National Laboratory in Livermore, California, has also developed a potent neutral oxime that readily enters the brain of guinea pigs. And Janice Chambers, a biologist at Mississippi State University in Starkville, together with her late husband, Howard Chambers, created a novel oxime with a fat-loving group that should help it traverse the blood-brain barrier. It alleviated symptoms in rats exposed to nerve agent surrogates and is undergoing further testing.
The likeliest nerve agent to be used in future attacks, defense experts say, is sarin. It's as volatile as water, disperses widely in the air, and doesn't linger, so attacking troops could enter a battlefield soon after its release. But soman, too, is a formidable threat. It evaporates only a fifth as quickly as sarin and therefore persists longer in the environment. Soman's tactical value "would be to deny the use of key terrain" by contaminating it, says Jonathan Newmark, a neurologist formerly with USAMRICD.
Soman's lightning-fast aging time means that oximes won't work against it. During the Gulf War, soldiers deemed at a risk of exposure out in the field proactively took pyridostigmine bromide, a drug used to treat a neuromuscular disorder called myasthenia gravis. It lodges temporarily in the AChE gorge, thwarting nerve agent binding. A countermeasure that has to be taken before exposure has obvious limitations: If terrorists were to get their hands on soman, they would almost certainly give no warning.