FREETOWN, Sierra Leone—Ebola continues to blindside us. We still know next to nothing about the virus. It resurfaced unexpectedly in Liberia in July, two months after the World Health Organization declared the outbreak there over. One leading hypothesis suggests Ebola re-emerged because the virus lurked in semen from a man who had survived the disease, then had unprotected sex.
How long does the virus reside in testes? One 1995 study on a single male suggested 82 days. Recent analyses suggest the same and sometimes longer: Four months, six months, even nine months. Can it linger in vaginal fluid or tears? No one knows for sure.
In fact, one of the only things proven by more than 13,000 people who have survived Ebola in the past year is that the disease is not over when it's over. Not for societies, and not for individuals. It seems miraculous when an Ebola survivor leaves a hospital, grasping an Ebola-free certificate, hugging loved ones through tears. If only the elation could last. Within weeks, many survivors suffer debilitating pain, surges of fever, encroaching blindness, unrelenting fatigue, hearing loss, depression, insomnia, migraines, and anorexia. Doctors cannot warn patients which of these symptoms will occur—if any—because they don't know.
"To emerge from an Ebola treatment unit is a remarkable thing, but it's a measured joy," says Ian Crozier, an American infectious disease doctor who contracted Ebola in Sierra Leone and was evacuated to Emory University Hospital in the Unites States. He survived, but he later experienced pain, obscured vision, hearing problems, and lapses in his short-term memory. He told me his brain scans show evidence of sustained damage.
Crozier's medical details were presented at a WHO conference on survivors held last month in Sierra Leone. There, Steven Yeh, one of Crozier's ophthalmologists at Emory Hospital, coolly clicked through slides describing the minutiae of Crozier's post-Ebola condition as if his patient weren't in the audience. He occasionally referred to Crozier as he was described in his medical records: as "Patient 3" and "a very tall man."
It's awkward, Crozier told me afterward at the conference reception. "I'm still learning how to be in this space," he said. "But I'm doing it because I'm convinced that what we learn at my bedside can be multiplied many times over, and I'm more interested in that than anything else."
Crozier is acutely aware of the contrast between the medical attention lavished on his every organ at Emory University Hospital and the lack of adequate health care for thousands of Africans who have been infected by Ebola. For example, the basic steroids currently used to treat pressure in survivors' eyes cost about $30 in Sierra Leone, but that's an expense few can afford, and some survivors will go blind as a result of not getting immediate treatment.
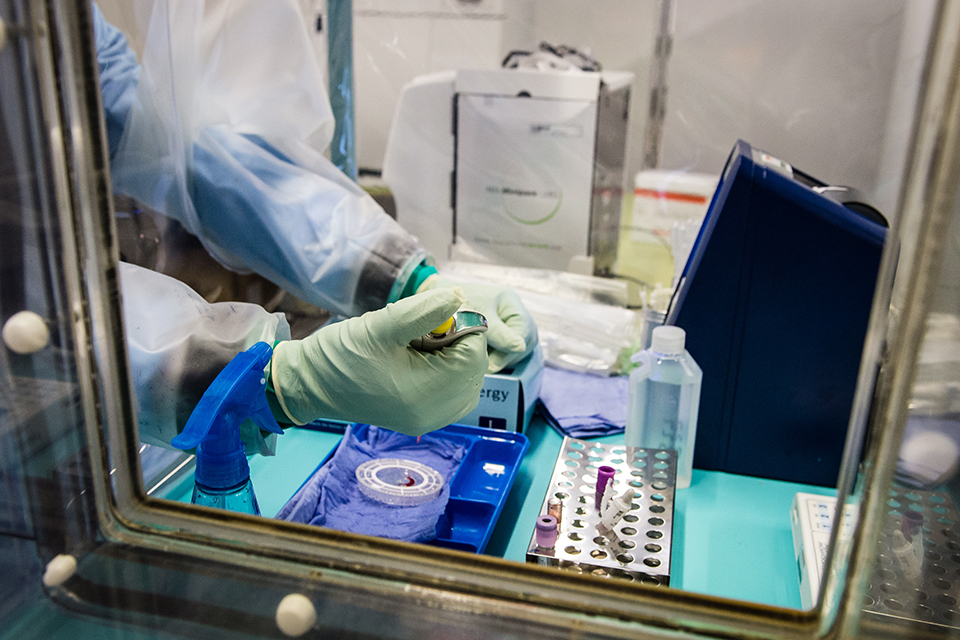
Similarly, a grassroots nonprofit group, the Sierra Leone Association of Ebola Survivors, is advocating for free, confidential tests to see whether their semen or other bodily fluids still harbor virus. But for now, even that test is out of reach.
A handful of clinics in each of the three hard-hit countries in West Africa offer free care to survivors in the surrounding community. At the WHO's meeting in Sierra Leone, the doctors from these clinics swapped notes on the percentages of survivors they see with various complaints. At a clinic in Guinea, for example, a third of survivors suffered abdominal pain; nearly half had difficulty concentrating; and all survivors reported feeling insecure, antisocial, and unaccepted by friends.
The doctors also debated which problems might be blamed on direct action of the virus, which on the body's inflammatory response, and which ailments attack survivors because their physical and emotional defenses are down. Sometimes survivors show up with symptoms that clinics eventually link to HIV, drug-resistant tuberculosis, manic depression, chicken pox, and more. During his presentation, Crozier advised his colleagues, "Expect the unexpected."
Then there are nonmedical pains. After the acute disease passes, many patients find themselves without jobs, without parents or spouses, and without shelter when landlords have evicted them from their homes. "Some survivors are now living in abandoned vehicles," said Kadiatu Fofanah, a member of the Sierra Leone Association of Ebola Survivors. "We need sustainable programs," she pleaded, such as education, employment, and housing. This desperation has grown this week as severe floods in Sierra Leone's capital displaced thousands.
Research on post-Ebola symptoms is needed to find better therapies now, as well as later. Ebola will inevitably strike again, as will the myriad post-Ebola conditions that may be preventable if treated pre-emptively. "Time is of the essence," Crozier said. "It's already too late for me." His vision returned after treatment, but now his hearing is impaired.
A month ago in eastern Sierra Leone, a laboratory technician named Mohamed S.K. Sesay, who had been infected by Ebola last year and survived, told me he'd happily volunteer to be a subject of study. "We need experts to come here," he said. "All of these complications, with vision, deafness, fevers, joint pain—they go on and off and on, and we don't want them to lead to permanent disabilities."
Sesay, a member of the Kenema Ebola Survivors Football Club, has become an advocate in his community. When aid organizations or the president of Sierra Leone pledge to offer free medicine, mental health care, food, and other provisions to survivors, Sesay passes on the hopeful messages. However, just as often, he breaks the news that aid is not coming after all. Ebola survivors "are always asking me, 'Where is the help?' " he explained. "I wish people would come and say, 'We don't have anything for you.' But the problem is there are a lot of promises—we will do this, we will do that—and nothing happens."
Sesay is a prime candidate for a program in development by Sierra Leone's government and the WHO, which involves employing health workers who survived Ebola to aid survivors in their communities. They would help ensure that survivors could take advantage of another government-led program in the works, a comprehensive care package. Mauricio Calderon, who leads the WHO's team on Ebola survivor care, says, "These advocates would assure that other survivors get appropriate and free health care in a timely fashion, and that medical consultations occur as needed." However, neither program has been rolled out on a nationwide scale. And because many symptoms appear to worsen without therapy, the burden grows with every day of delay. What's more, the loss of employment and education due to sickness can lead to a downward spiral of nearly inescapable poverty.
Despite the urgency of survivors' situations, some humanitarian agencies seem more interested in using survivor plights to raise funds rather than to help individuals. For example, this summer, the United Nations Development Programme released a virtual reality film on Ebola survivors, to be viewed by people in rich countries. A communications officer at UNDP called the film "expensive" but would not reveal its price. Even if the film raises funds for the U.N., the donations certainly won't manifest in the form of care for survivors as quickly as they're needed. And because U.N. agencies refuse to reveal their budgets, I can't say how many medicines for survivor ailments might have been purchased now instead of a virtual reality film, or how many health advocates paid, or how much shelter for needy survivors might have been established.
The U.S. and international doctors at the WHO's meeting were well aware of survivors' urgent needs. They have been pushing donors and policymakers to continue the fight against Ebola, even though the dramatic peak of the contagion has passed.
"People ask me how I feel about the fact that I got evacuated [out of Sierra Leone], and I can be truthful and say I would have been dead in a week had I not been," Crozier told me. "So I'm grateful for the opportunity, but at the same time, I'm haunted by the fact that so many of my patients and local colleagues died because they did not have the same access, and that reflects long-standing inequalities in global health. So, since I have the opportunity to speak for more than myself, I'm going to use it."