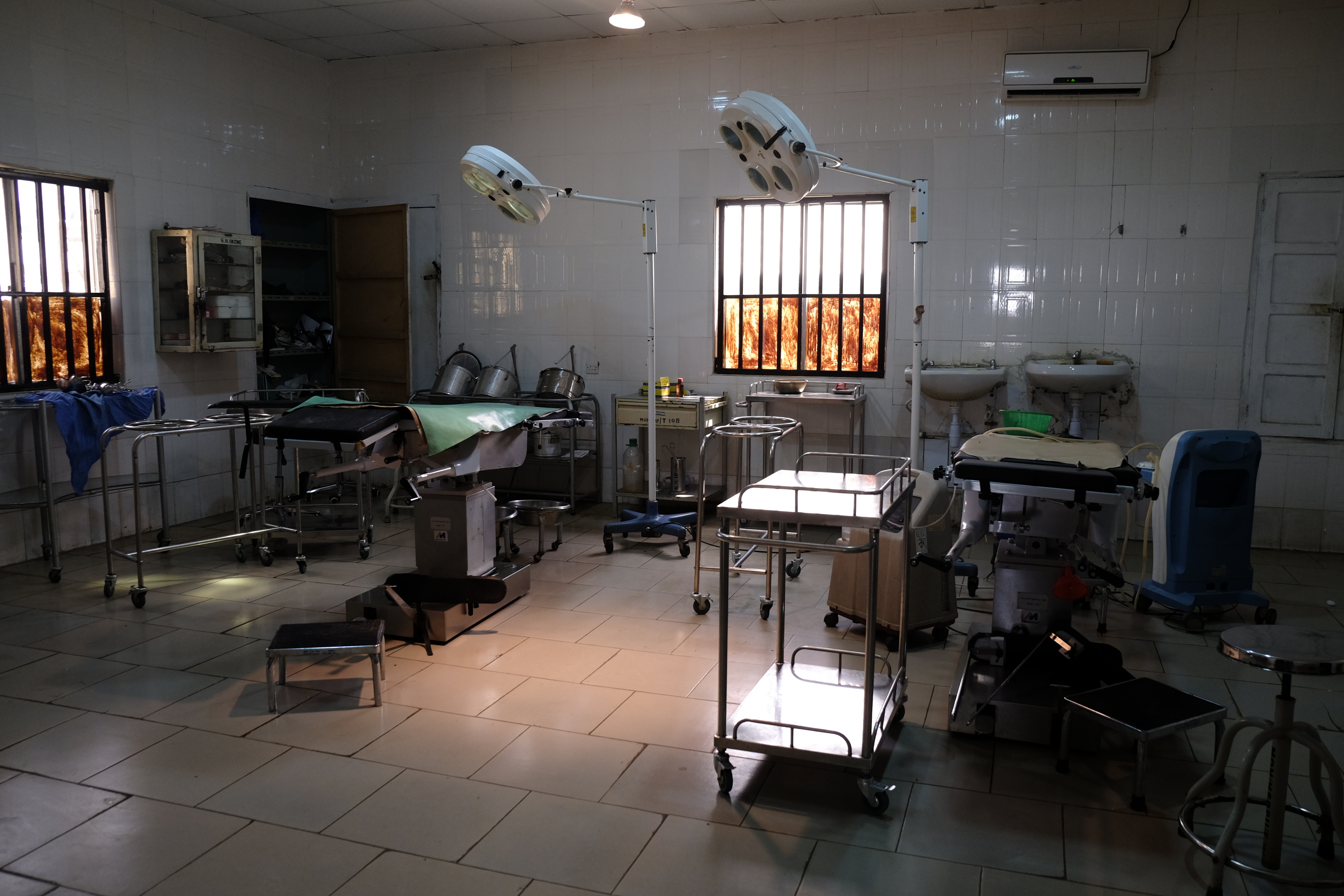
At the Okene Zonal Hospital in Kogi State, Nigeria, an infant's tiny face—still flecked with a newborn patina because the boy had been born less than an hour earlier—was barely visible. The baby, wrapped in billows of Ankara cloth, lay on a small mattress inside a slatted metal basket whose graceful curves evoked a Victorian-era birthing implement, a basket that had likely been in continuous use since the hospital opened in 1960, the year Nigeria became independent.
Despite the heat of the mid-July rainy season, the deputy ward matron dressed the child in a terrycloth jumpsuit, booties, and a large winter hat. Then she triple-gloved her hands and, holding the baby's recently cut umbilical cord stump in her left hand, spread a thick layer of chlorhexidine gel along the length of the stump.
The infant was lucky on at least two counts. First, in a country where the minister of health tweets about Nigeria's "broken health system"1 and the neonatal mortality rate is among the highest in the world, the child happened to be born in one of a handful of Nigerian states making a concerted effort to promote the use of chlorhexidine gel, a low-cost intervention that instantly reduced his chances of dying from the sort of massive infection that in Nigeria and other developing countries can all too easily take root in a newborn's umbilical cord stump.
Read the full text article on the Health Affairs website.