KONO, Sierra Leone — A recent two-week visit to Kono, a remote and rural district in Sierra Leone, showed that trust is at the heart of a nonprofit's effort to combat not only the spread of Ebola but the world's worst infant mortality rate.
There, a small nonprofit called the Wellbody Alliance is grappling with the loss of trust caused by the Ebola epidemic, and working to rebuild that trust with a bold new program.
New research shows that outreach efforts from government institutions, not the independent nonprofits known as NGOs, are most effective at building trust in government. But in Sierra Leone, where the government is experiencing political turmoil and known best for its seemingly intractable culture of corruption, many NGOs are acting with more independence because the stakes are so high.
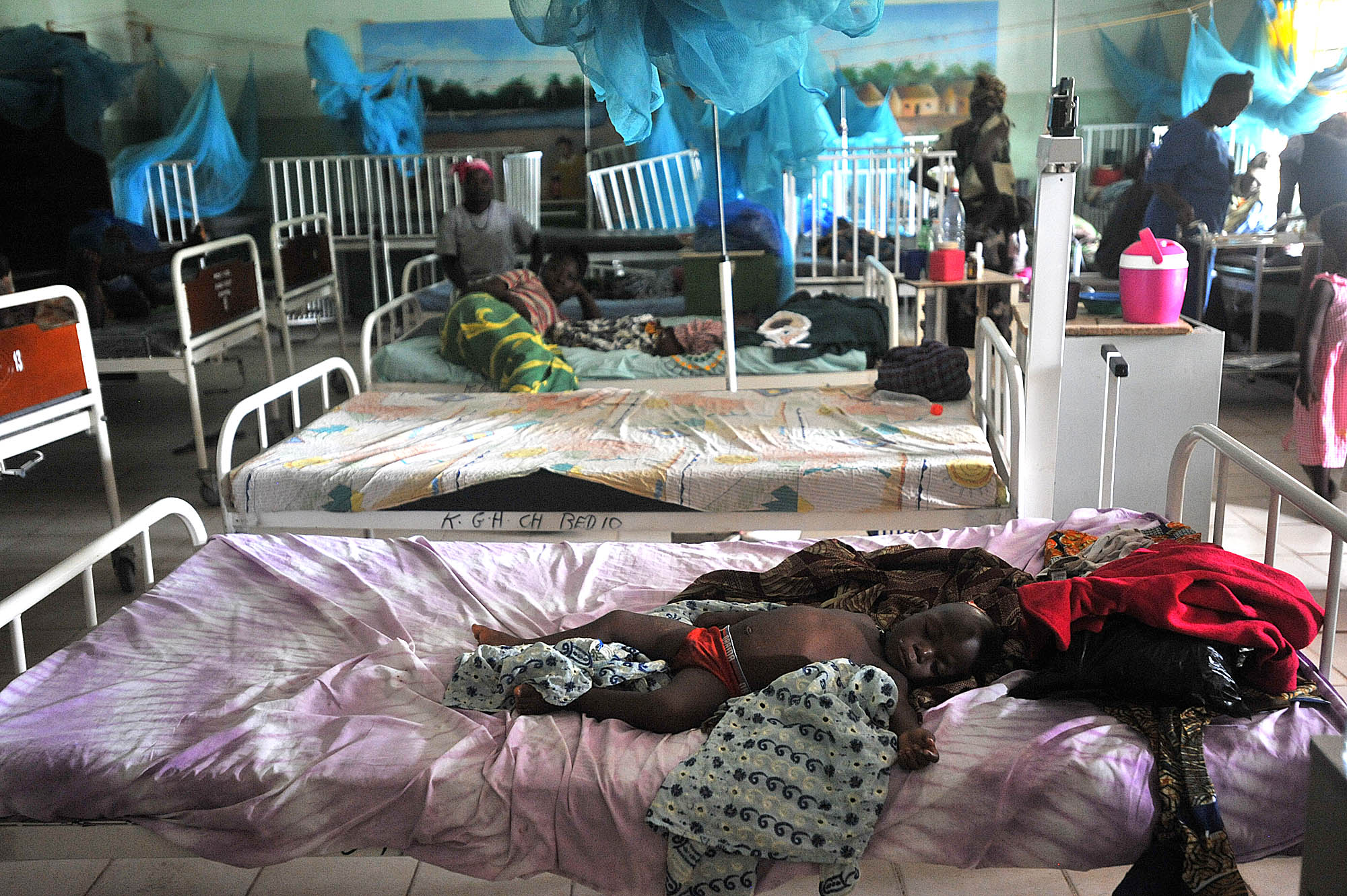
One in five Sierra Leonean children die before their fifth birthday. In Kono, where many live in mud huts without electricity or running water, scraping by on an income of less than a dollar a day, the rate is likely higher.
There are many poverty-driven causes behind the deaths of most infants and young children: doctor shortages, insufficient government support, corruption and lack of medical resources are among them.
But for Wellbody, a small NGO with offices in Boston and Sierra Leone, one of the biggest obstacles is a lack of trust between the medical community and pregnant women. For nearly nine years, Wellbody has operated a local health clinic, a white-walled concrete building with blue trim and lettering that draws a crowd of several dozen every day by 8 a.m.
Like other health care providers in the region, Wellbody struggled to maintain its relationships with the community during the Ebola epidemic, which saw cases of patients fleeing from treatment centers, villagers establishing barriers to block ambulances, and a dramatic plunge in patient attendance.
Those incidents reflected a deep cultural division between the medical community and the people, most of whom identify as Muslims or Christians but also believe in traditional magic-based cures.
Medical staff, including those at Wellbody, expressed their distrust of those spiritual beliefs, which are often espoused by traditional birth attendants.
Boyama Gladys Kacingor, a midwife who works for Wellbody, described some of the drawbacks of at-home births.
"Traditional attendants, they can deliver a woman anywhere," she said. "They don't think of the hygiene. Whether the place is clean or not, as long as the woman is ready to deliver, they do it."
Scientists and Westerners often find it easy to make fun of traditional healers, said Storm Portner, community co-manager for Wellbody.
"You hear, in the meetings in public health circles, that there's a lot of disdain for traditional practices," Portner said.
But Wellbody's leadership says the key to gaining the trust of the local population doesn't lie in trying to marginalize a birthing system that's been in place for thousands of years.
In fact, said Portner, many traditional healers have valuable lessons for professionally trained health care workers at places like Wellbody.
"They offer a deep understanding of the people here, and the care that they want," he said.
In order to harness the advantages traditional healers have, Wellbody is implementing an unusual plan. Rather than competing with the healers, they put them on the payroll.
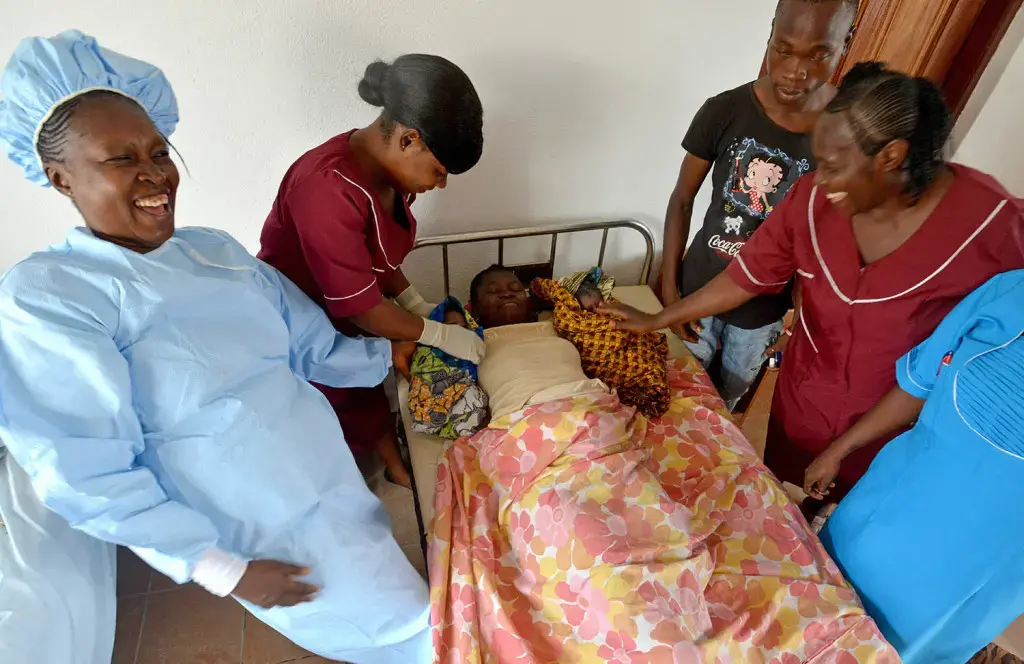
Over the past several months, Wellbody has hired a total of 10 well-respected women who have collectively delivered thousands of babies in the villages surrounding the clinic. The clinic opened a new delivery center on April 1.
The women, whose existing knowledge base is supplemented with medical training, work to deliver babies with a team that includes medically trained nurses.
Kacingor explained how she handles a situation in which a traditional attendant might want to administer an herbal remedy to a woman whose labor is slow.
"We don't shout at them or talk to them in a way that they do not like. We just talk to them politely," she said. "I would tell the (birth attendant) two things do not go together. This woman has been under my care. She has been taking drugs which I hope are still working into the system. If I allow you now to give her this, it is an overdose. Anything can happen. If something bad happens, I will be blamed."
Wellbody expects that this approach will help to build strong relationships with the attendants, which will extend to trusting relationships with the community at large.
Benjamin Morse, a Colby College graduate who has spent much of the past year in West Africa, said he had no direct knowledge of the clinic, but he supports the concept.
"If this offers an option to citizens to have the safety of Western medicine without breaking cultural traditions, that's a win," said Morse, who has been conducting surveys on the spread of Ebola in the region.